Signalment:
2 year old Thoroughbred colt (
Equus caballus)The horse was normal and trained as usual
the previous day, but did not consume all of his feed the night prior. The referring
veterinarian examined the horse at 11 AM; the temperature was 104.8°F, the heart
rate was elevated, and he was reluctant to move. He was treated with Banamine
and Bactrim. The horse died spontaneously at 3:30 PM, at which time bloody
froth was expelled from both nostrils.
Gross Description:
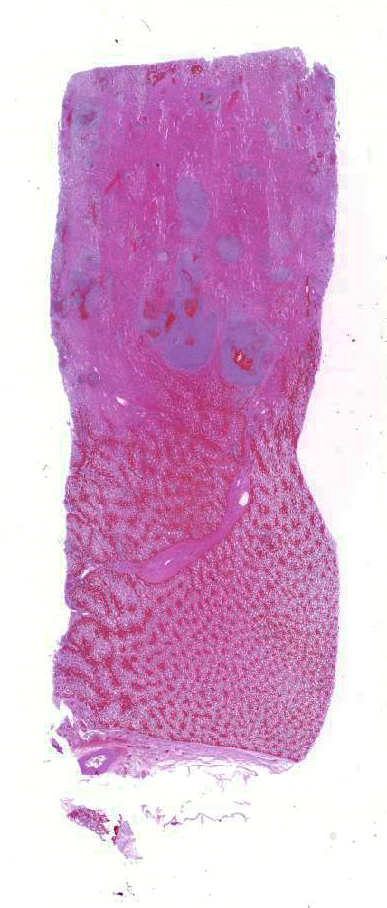
The kidneys are bilaterally markedly
enlarged. The right kidney weighs 1.85 kg and measures 20 x 19 x 8.5 cm, and
the left kidney weighs 1.86 kg and measures 24.5 x 16 x 7 cm (each kidney is
approximately 0.42% of body weight; 0.25% is normal). Bilaterally, the
perirenal adipose tissue is mildly edematous. There are widespread multifocal,
slightly raised, 1 to 10 mm diameter, tan-yellow foci on the subcapsular
surface of both kidneys which occasionally bulge from the capsular surface. The
discoloration frequently ex-tends into the renal capsule and oc-casionally into
the perirenal adipose tissue. The capsules are friable and difficult to peel.
Both kidneys moderately bulge on cut surface, and the cortices contain myriad
1mm diameter to 9 x 2 mm yellow-tan foci which occasionally have a cavitated
center.
Histopathologic Description:
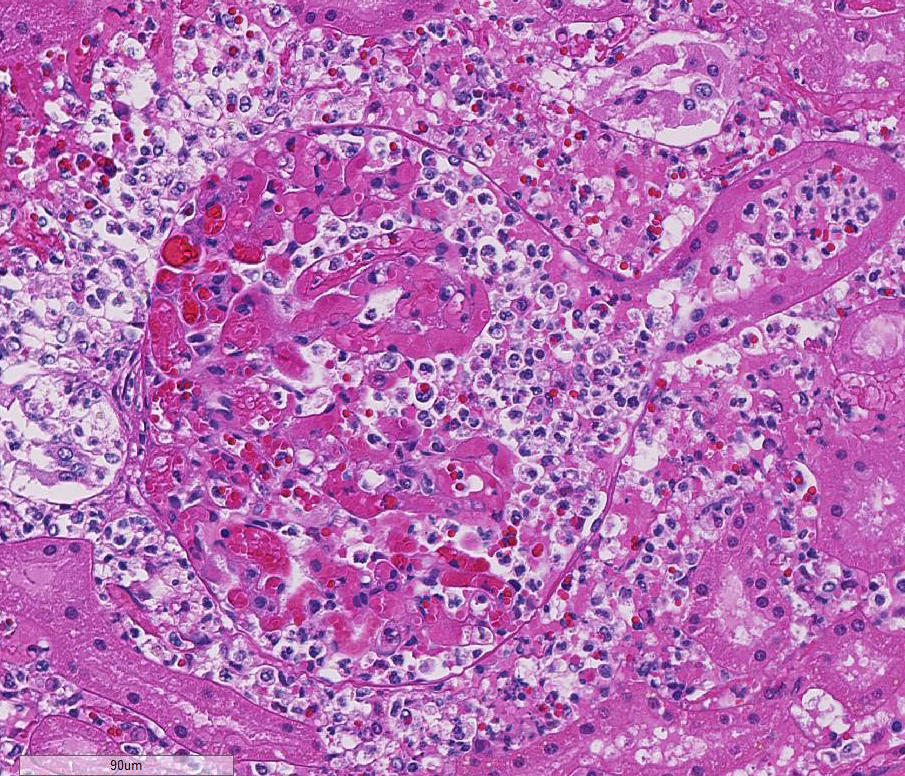
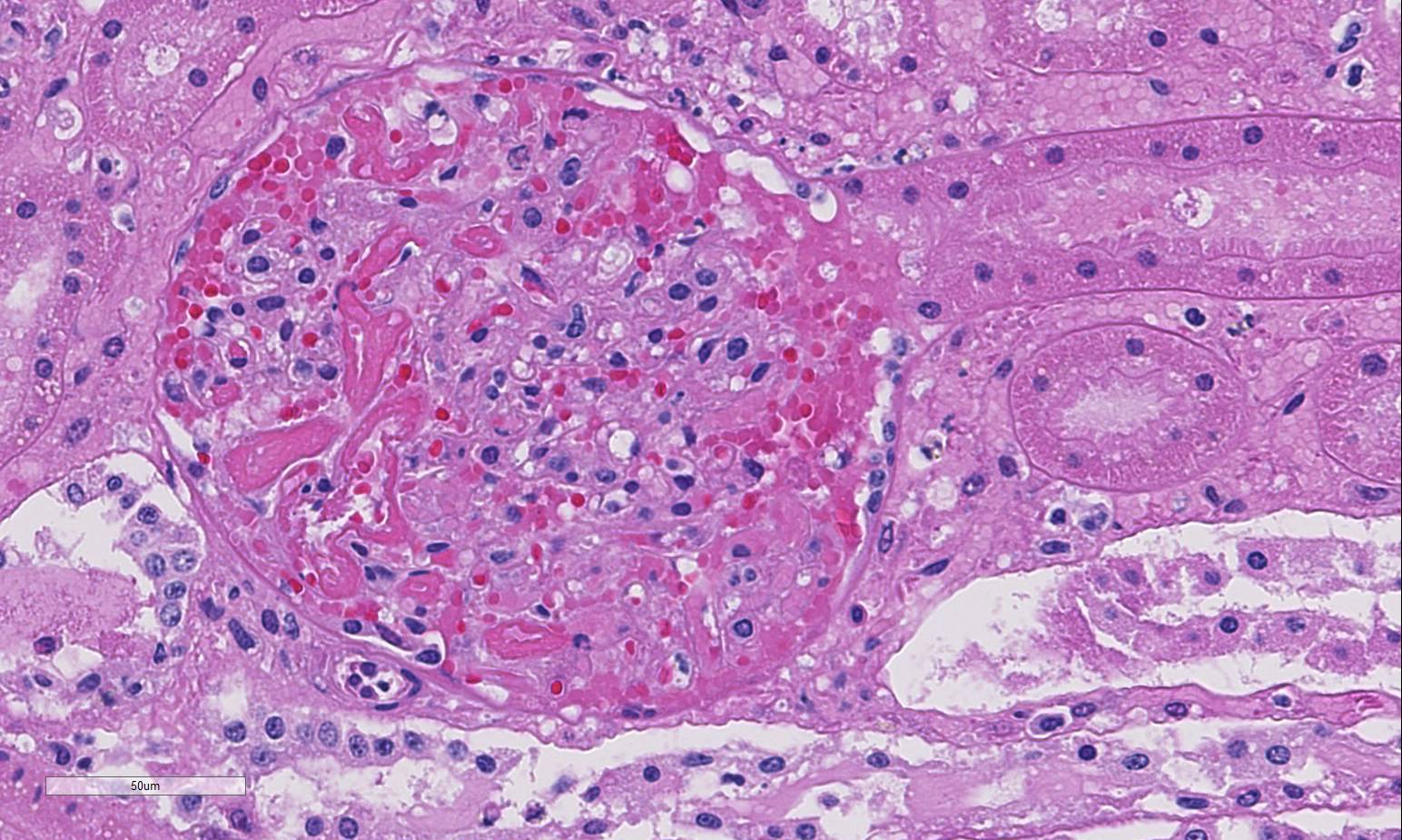
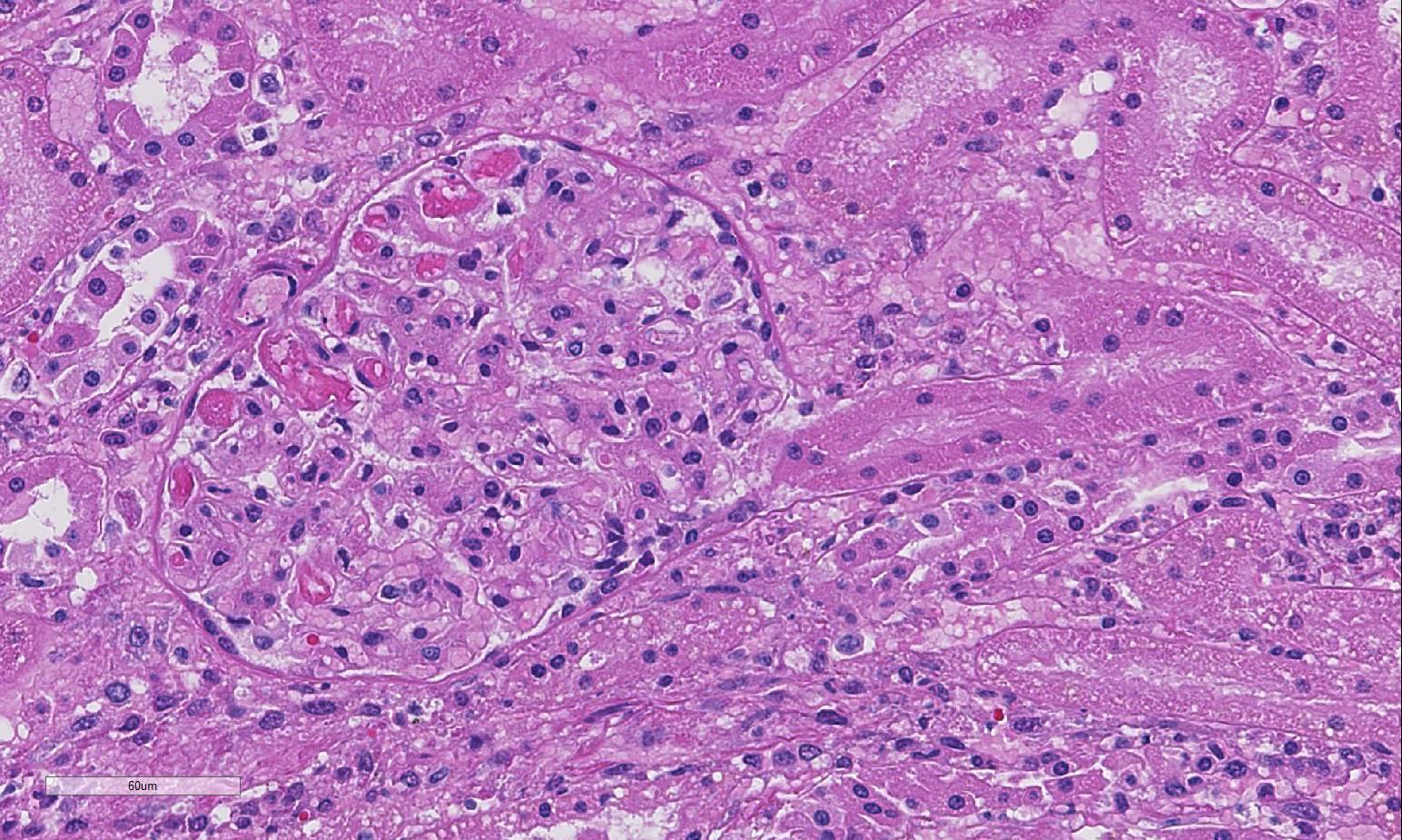
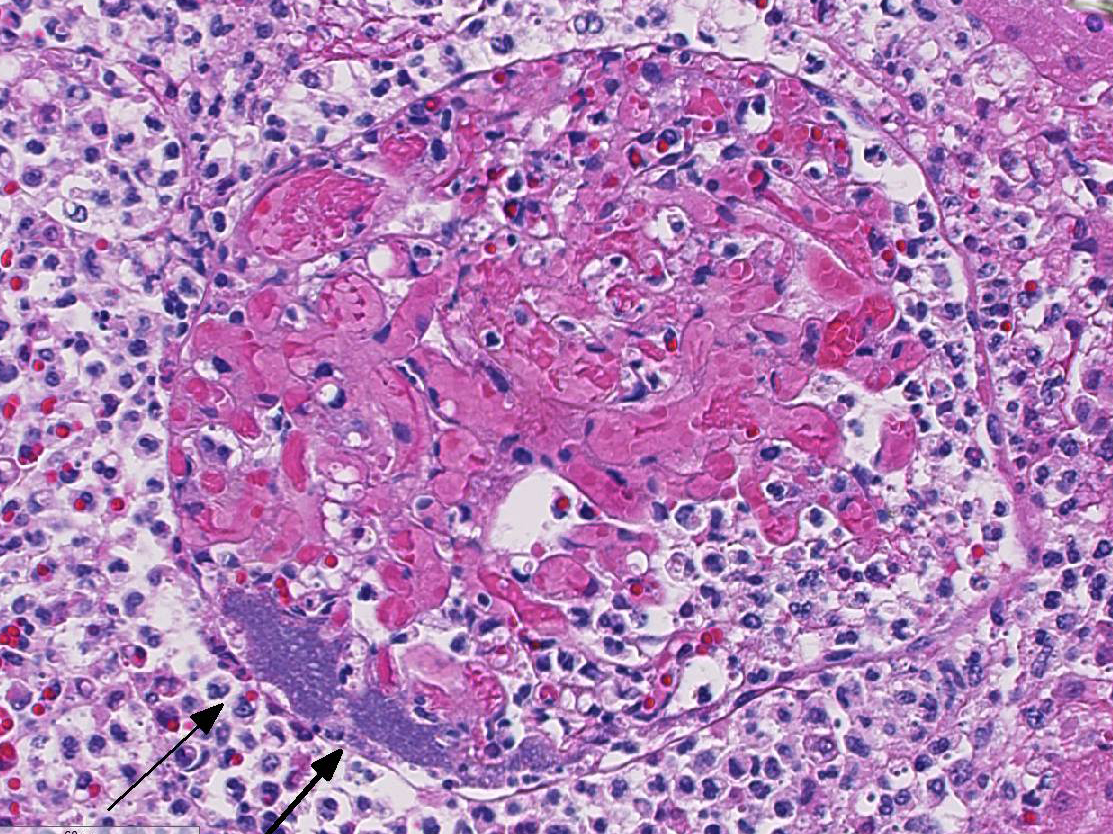
Predominantly in the cortex, there are multifocal to coalescing,
nodular in-flammatory infiltrates predominantly of degenerate neutrophils,
fewer macrophages, and cellular debris. This infiltrate is often centered on
glomeruli, extending into and sometimes effacing the adjacent interstitium and
renal tubules. Renal tubules in inflamed areas are sometimes degenerate or
necrotic. Larger blood vessels sometimes contain luminal aggregates of fibrin,
degenerate and viable neutrophils, cellular debris and erythrocytes;
inflammation often extends into the vessel wall (vasculitis). Many foci of
inflammation contain aggregates of gram-negative bacilli.
Morphologic Diagnosis:
Embolic
nephritis, suppurative, acute, multifocal to coalescing, severe, with in-tralesional
gram-negative bacilli and vasculitis.
Lab Results:
Microbiology:
Aerobic culture of the kidney yielded
heavy growth of Actinobacillus equuli ssp. equuli.
Condition:
Actinobacillus equuli
Contributor Comment:
The
most frequently isolated agent in equine cases of embolic nephritis is Actinobacillus
equuli, most often secondary to septicemia of foals.4 A.
equuli is a gram-negative bacillus that can be normal flora of the oral
cavity, reproductive tract and intestinal tract of horses.2,5 It is
especially known for its tendency to create microabscesses in the kidneys and
other organs.4 In foals, A. equuli typically causes
septicemia, also known as sleepy foal disease.2 Septicemic lesions
typically include embolic lesions in the kidney, lungs and liver, with lesions
also reported in the umbilicus, adrenal gland, and joints.2 In
adult horses, A. equuli has been reported to cause sepsis, nephritis, en-docarditis,
pericarditis, peritonitis, en-teritis, pleuropneumonia, arthritis, pe-riorchitis,
and abortion.2,3,5 A. equuli infections in adult horses are
thought to be predisposed by stress or other infections, such as respiratory
viruses or salmonellosis.2
JPC Diagnosis:
Kidney: Nephritis, embolic, suppurative, multifocal, marked with necrotizing vasculitis
and colonies of bacilli.
Conference Comment:
Actinobacillosis in adult horses is uncommon and most frequently
associated with an underlying disease. There are two subspecies of
A.
equuli, a hemolytic subspecies termed
A. equuli subsp
.
haemolyticus which is isolated from the normal oral cavity and respiratory
tract, and a non-hemolytic form termed
A. equuli subsp
. equuli,
which also resides in the oral cavity as well as the gastrointestinal tract of
adult horses and is the agent of septicemia in foals.
1 The hemolytic
form has been associated with various infections including peritonitis,
reproductive failure and respiratory disease. The bacterium possesses an RTX
exotoxin known as Aqx that is cytotoxic to equine red blood cells. The
non-hemolytic subspecies is more commonly present in cases of septicemia and
may also be associated with respiratory disease, embolic nephritis and
infection in other organs as well.
1 In septicemic cases,
Actinobacillus
can act as the primary agent or be a secondary infection following other viral
or bacterial infections. The presence of endotoxin likely plays a role in the
endothelial damage, vasculitis and bacterial emboli which are classically seen
in septicemic cases. Although most often associated with foals in conjunction
with events such as failure of passive transfer, septicemic lesions such as
embolic nephritis, as seen in this case, as well as pneumonia, may be seen in adult
horses.
1 In cases of embolic nephritis,
bacteria become lodged in glomerular capillaries resulting in the presence of
suppurative lesions or abscesses and, in some cases, when emboli are large
enough, may occlude arteries resulting in septic infarcts. In septicemic foals
that survive for a period of time, microabscesses will be seen in multiple
organs and polyarthritis will be present.
A. equuli may also cause
diarrhea and hemorrhagic enteritis in foals. A common agent of embolic
nephritis in swine, perhaps the most common, is
Erysipelothrix rhusiopathiae;
in cattle the common agent is
Trueperella pyogenes; and in sheep and
goats
Corynebacterium pseudotuberculosis may be associated with embolic infections.
1
Although uncommon,
A. equuli infection can be associated with
endocarditis or myocarditis in adult horses
6 and has also been
associated with reproductive losses.
Conference participants
described the prolific inflammatory infiltrates as being centered on vessels as
well as effacing glomeruli, with adjacent tubules being secondarily affected
with varying severity. Tubules are multifocally ectatic and variably contain
necrotic, sloughed tubular epithelial cells admixed with fibrin, hemorrhage and
proteinaceous fluid. Fibrin thrombi with colonies of coccobacilli are
occasionally seen in glomerular tufts. Some conference participants
interpreted the most severely affected area of the cortex as coagulative
necrosis secondary to infarction due to fibrin thrombi; others attributed the
tinctorial change as more consistent with some degree of autolysis.
7The
differential diagnosis discussed by participants in the case of this horse
included
Escherichia coli,
Klebsiella sp.,
Streptococcus
sp.,
Rhodococcus equi and
Salmonella species.
References:
1. Cianciolo RE, Mohr FC. Urinary System
. In:
Maxie MG, ed. Jubb, Kennedy, and Palmer's Pathology of Domestic Animals.
6th ed. Vol 2. St. Louis, MO: Elsevier; 2016:432-433.
2. Layman
QD, Rezabeck GB, Ramachandran A, Love BC, Confer AW. A retrospective study of
equine actinobacillosis cases: 1999-2011. J Vet Diagn Invest. 2014; 26(3):365-375.
3. Matthews
S, Dart AJ, Dowling BA, Hodgson JL and Hodgson DR. Peritonitis associated
with Actinobacillus equuli in horses: 51 cases. Aust Vet J.
2001; 79(8): 536-9.
4. Maxie,
MG, Newman SJ. Urinary System. In: Maxie MG, ed. Jubb, Kennedy, and
Palmer's Pathology of Domestic Animals, 5th ed. Vol 2. Edinburgh:
Elsevier Saunders. 2007:479-480.
5. Patterson-Kane
JC, Donahue JM and Harrison LR. Septicemia and peritonitis due to Actinobacillus
equuli infection in an adult horse. Vet Pathol. 2001; 38(2): 230-2.
6. Robinson WF, Robinson NA. Cardiovascular system. In:
Maxie MG, ed. Jubb, Kennedy, and Palmer's Pathology of Domestic Animals.
6th ed. Vol 3. St. Louis, MO: Elsevier; 2016:31-42.
7. Uzal FA, Plattner BL, Hostetter JM. Alimentary System. In:
Maxie MG, ed. Jubb, Kennedy, and Palmer's Pathology of Domestic Animals.
6th ed. Vol 2. St. Louis, MO: Elsevier; 2016:114.