Signalment:
Gross Description:
Further findings included a severe necrotising pneumonia and splenitis, a generalized hyperplasia of the lymph nodes and severe follicular hyperplasia of the spleen.Â
Histopathologic Description:
Transmission electron microscopy of skin samples revealed single orthopox like particles in the cytoplasma of keratinocytes.Â
Monkey pox virus was diagnosed by PCR and cell culture.
Morphologic Diagnosis:
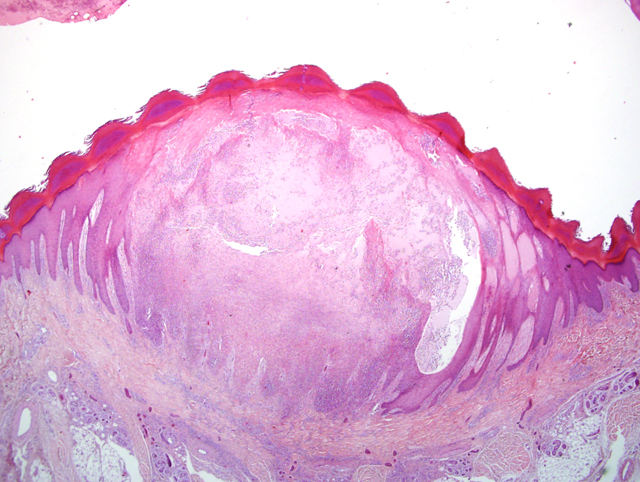
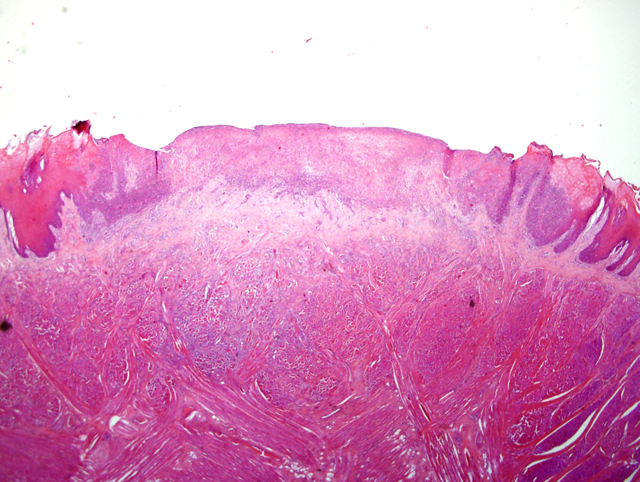
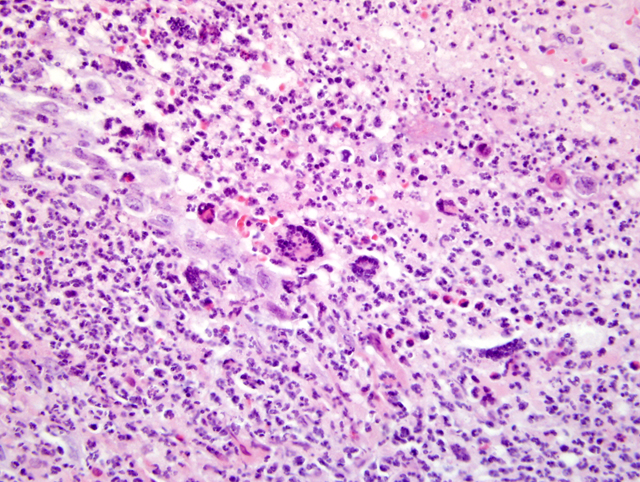
Tongue: Dermatitis, erosive-ulcerative, subacute, multifocal, severe, with single intracytoplasmatic eosinophilic inclusion bodies, rhesus macaque (Macaca mulatta), non-human primate.
Skin: Dermatitis, proliferative, pustular, subacute, multifocal, severe, with single eosinophilic intracytoplasmatic basophilic inclusion bodies and rare syncytia, rhesus macaque (Macaca mulatta), non-human primate.
Lab Results:
Immunohistochemistry: Herpes simplex Type 1 and 2: negative
Condition:
Contributor Comment:
Monkeypox virus belongs to the orthopox virus group of pox-viruses. Other orthopox viruses that can cause infection in humans and non-human primates include variola (smallpox), vaccinia (used in smallpox vaccine), and cowpox viruses. Pox-viruses are large, complex double stranded DNA viruses.Â
Naturally monkeypox virus only occurs in the tropical rain forest of Western and Central Africa, where it causes subclinical endemic infections in several non-human primate (NHP) species. In the past outbreaks have been reported in captive NHPs, primarily rhesus and cynomolgus, involving institutes importing large numbers of macaques. But the disease has also been reported in marmosets, squirrel monkeys, langurs, baboons, orangutans, gorillas, gibbons and chimpanzees.6,7,10 The first human case of monkeypox was reported in 1970. Till then several human cases of monkeypox appeared in the tropical rain forest areas of West and Central Africa as isolated cases or as small epidemics. In these regions the infection causes a serious, sometimes fatal smallpox-like disease among young people. Transmission occurs probably aerogenously, by biting or other contacts. People can get monkeypox from an infected animal through a bite or direct contact with the infected animals blood, body fluids, or lesions (bush meet problem). In 2003 monkeypox was reported among several residents in the United States who became ill after having contact with sick imported prairie dogs. The disease can be spread from person to person too, but it is much less infectious than smallpox.
In non-human primates the disease in usually exhibit a high morbidity and low mortality. Clinical signs may be inapparent or animals may exhibit fever, lymphadenopathy and cutaneous eruptions. Death is uncommon except in infant monkeys. Typical pocks appear as papules of 1 to 4 mm in diameter, which then develop into pustules containing cell debris. The pustules become umbilicated and covered by crusts. The most common sites of pock formation in the monkeys are the face, hands and feet, the mucous membranes of the oral cavity and the genital tract, but also pharynx, larynx trachea, lung, spleen and lymph nodes are commonly involved.
Today we gained experience with the outcome of the disease in immunocompromised monkeys. This accidental case of monkeypox in an immunocompromised animal described here showed that the disease outcome was characterized by severe vesicular exanthema. The skin rash was accompanied by severe respiratory tract involvement and progression of the disease was fatal. Till now it is not clear how transmission occurred in this case. Diagnosis was complicated due to the minimal content of inclusion bodies indicative for poxvirus infection. By electron microscopy typical orthopox like viral particles were demonstrable. An Eczema herpeticatum was considered as differential diagnosis, but immunohistochemistry for Herpes simplex type 1 and 2 was negative.Â
JPC Diagnosis:
2. Haired skin: Dermatitis, necroulcerative, neutrophilic and eosinophilic, focally extensive, severe with ballooning degeneration.
3. Tongue: Glossitis, necroulcerative, neutrophilic and eosinophilic, multifocal, marked, with ballooning degeneration and intralesional cocci (Fig. 4-2 and 4-3).
Conference Comment:
Ultrastructurally, orthopox viruses are 375 X 200 nm particles, located free in the cytoplasm, composed of an outer membrane enclosing a characteristic dumbell-shaped inner electron lucent core that is bounded by two lateral bodies.4
Table extracted from Ginn et al.3
| Orthopoxvirus | Key points |
| Camelpox virus | Dromedary camels; clinically identical to camel contagious ecthyma (parapox) |
| Cowpox virus | Cutaneous and occasionally respiratory lesions in domestic cats; on face and forepaws; affects wild and domestic Felidae, cattle, dogs, rodents, humans; not endemic in cattle, and infections in cattle are uncommon; wild rodents are the reservoir; severe fatal pneumonia in elephants |
| Ectromelia virus (mousepox virus)8 | Limb amputation in surviving mice; systemic infection |
| Monkeypox virus | Rodents, New World monkeys, and great apes; systemic disease |
| Buffalopox virus | Affects waterbuffalo in India; Zebu cattle apparently refractory to infection; closely related to Vaccinia virus |
| Uasin Gishu disease virus (unassigned) | Horsepox became naturally extinct in 19th century; recent uncharacterized orthopox viruses isolated from horses with equine papular dermatitis, and in equines with Uasin Gishu disease in Kenya; are found closely related to Vaccinia virus and cowpox virus |
| Vaccinia virus | Does not cause natural infection in domestic animals |
| Variola virus (human smallpox) | Affects humans and non-human primates; irradicated? |
References:
2. Bernard SM, Anderson SA: Qualitative assessment of risk for monkeypox associated with domestic trade in certain animal species, United States. Emerg Infect Dis 12:1827-1833, 2006
3. Ginn PE, Mansell JE, Rakich PM: Skin and appendages. In: Jubb, Kennedy, and Palmers Pathology of Domestic Animals, ed. Maxie MG, 5th ed., vol. 1, pp. 664-674. Elsevier Limited, St. Louis, MO, 2007
4. Langohr IM, Stevenson GW, Thacker HL, Regnery RL: Extensive lesions of monkeypox in a prairie dog (Cynomys sp.). Vet Pathol 41-702-707, 2004
5. M+�-�tz-Rensing K, Ellerbrok H, Ehlers B, Pauli G, Floto A, Alex M, Czerny CP, Kaup FJ: Fatal poxvirus outbreak in a colony of new world monkeys. Vet Pathol 43:212-218, 2006
6. McConnell SJ, Hickman RL, Wooding WL, Huxsoll DL: Monkey pox: Experimental infection in chimpanzees and immunization with vaccinia virus. Am J Vet Res 29:1675-1680, 1968
7. Marennikova SS, Shelukhina EM, Maltseva VI, Ladnnyj ID: Poxviruses isolated from clinically ill and asymptomatically infected monkeys and a chimpanzee. Bull WHO 46:613-620, 1976
8. Percy DH, Barthold SW: Mouse. In: Pathology of Laboratory Rodents and Rabbits, 3rd ed., pp. 25-28. Blackwell Publishing, Ames, IA, 2007
9. Peters JC: An epizootic of monkey pox at Rotterdam Zoo. Int Zool Yearb 6:274-275, 1966
10. Von Magnus P, Andersen EK, Petersen KB, Birch-Anderson A: A pox like disease in cynomolgus monkeys. Acta Pathol Microbiol Scand 46:156-176, 1959