Joint Pathology Center
Veterinary Pathology Services
Wednesday Slide Conference
2018-2019
Conference 5
Sept 26th, 2018
CASE III: 13749 (JPC 4033383-00).
Signalment: 7-month-old B6;129 wild type mice (hybrid C57BL/6J; 129X1/SvJ), male.
History: The mouse belonged to a WT +/+ control group in a study using genetically engineered mice on a B6;129 background. It was euthanatized at the age of 7 months for ethical reasons due to a rapidly growing submandibular mass. No other animal of the study was affected.
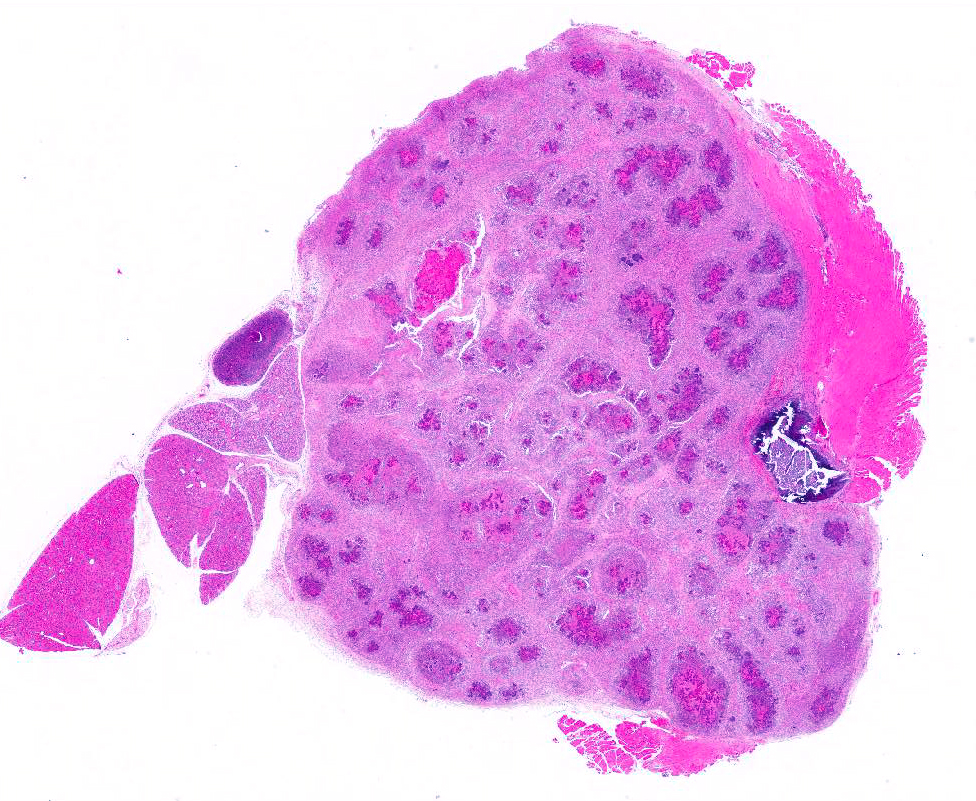
Gross Pathology: A multinodular tan mass replaced and destroyed most of the left submandibular salivary gland. After section the mass, measuring 2cmx1cm, appeared encapsulated and filled with white to tan caseous material.
Laboratory results: None provided.
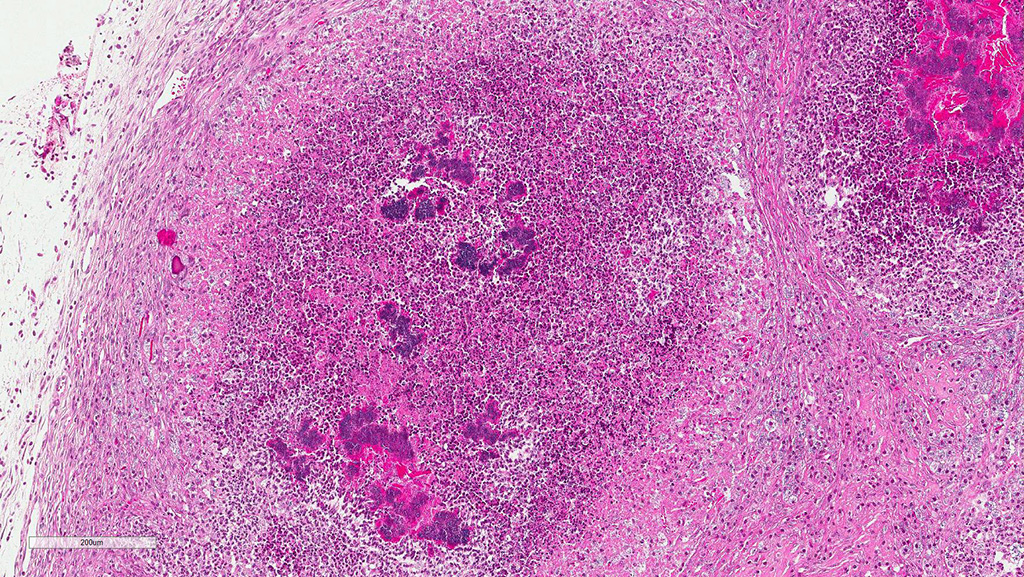
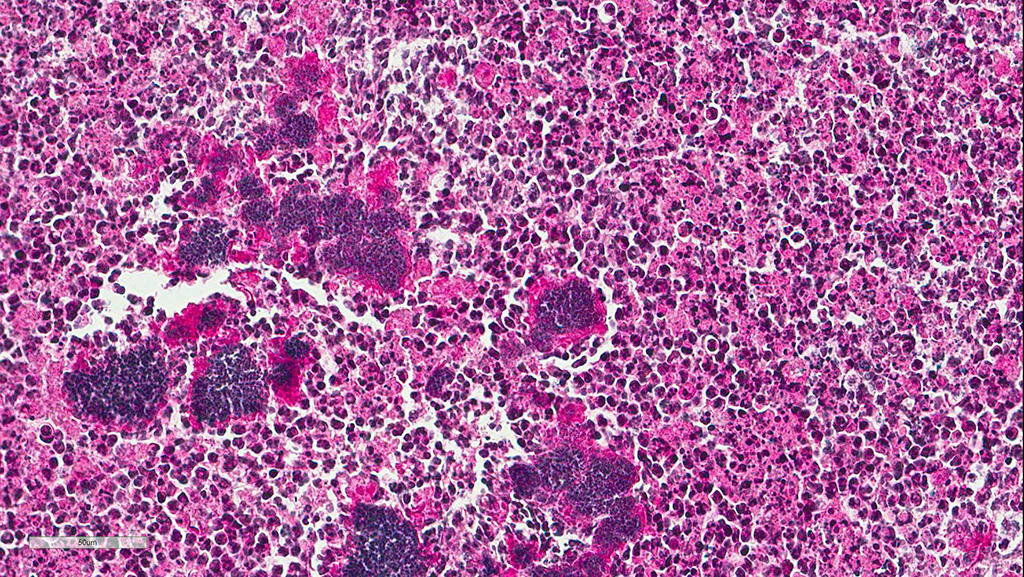
Microscopic Description: The submandibular salivary gland is almost entirely replaced by a well-circumscribed multifocal coalescing inflammatory lesion. Most foci are identical and centered on a core of eosinophilic karyolitic or karyorrhectic necrotic cell debris, pyknotic and karyorrhectic neutrophils (suppuration) and cocci colonies circumscribed by a radiating band of hyaline eosinophilic material (Splendore-Hoeppli phenomenon). A peripheral rim of activated macrophages, epithelioid macrophages, multinucleated giant cells, lymphocytes, fibroplasia and fibrosis form the external limit of those pyogranulomas. Macrophages and giant multinucleated cells often display a markedly enlarged cytoplasm filled with myriads of cocci. Those bacteria-filled macrophages are also observed within the fibrotic bands. Necrotic centers display multifocal dystrophic mineralization.
Eosinophilic macrophages and acicular or rectangular eosinophilic birefringent crystals are observed within the pyogranulomas. Crystals are found free in the extracellular space and less commonly in the cytoplasm of activated macrophages and giant cells.
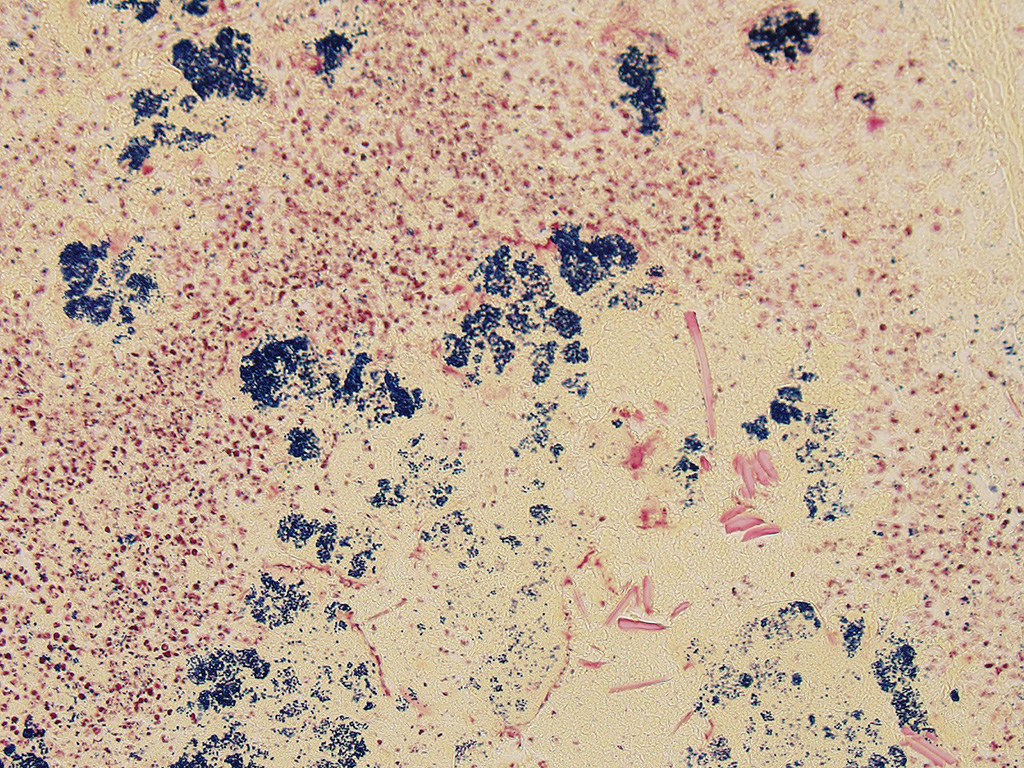
A Gram coloration was performed and revealed the presence of abundant gram-positive cocci, 1 to 2 um in diameter, consistent with staphylococci.
Contributor’s Morphologic Diagnoses: 1. Multifocal coalescing chronic pyogranulomatous sialoadenitis with cocci circumscribed by Splendore-Hoeppli phenomenon (botryomycosis).
- Presence of acicular and rectangular eosinophilic crystals into macrophages, giant cells, and extracellular space.
Contributor’s Comment: Botryomycosis is a chronic suppurative infection characterized by a granulomatous inflammatory response to bacterial pathogens; it may present with cutaneous or, less commonly, visceral involvement. The term botryomycosis is derived from the Greek word botrys (meaning "bunch of grapes") and mycosis (a misnomer, due to the presumed fungal etiology in early descriptions). In Human, the major etiologic agent of botryomycosis is Staphylococcus aureus (40%) followed by Pseudomonas aeruginosa (20%), coagulase-negative staphylococci, Streptococcus spp, Escherichia coli, and Proteus spp1. The Spendore-Hoeppli phenomenon consists of antigen-antibody precipitates, immunoglobulin G, C3 complement, tissue debris and fibrin1.
Staphylococci are commensal bacteria that inhabit the skin and mucous membrane and that can become pathogenic under certain circumstances. In the mouse, disease has been associated with Staphylococcus aureus and S. xylosus, causing necrotizing dermatitis, chronic suppurative infection of cutaneous adnexae, conjunctiva, periorbital tissues, preputial glands and regional lymph nodes2. The Splendore-Hoeppli phenomenon is classically observed in staphyloccocal lymphadenitis2 and in chronic skin infection affecting immune compromised mice such as agammaglobulinemic or nude mice3. Botryoid abscess of a salivary gland is to our knowledge uncommon, especially in immunocompetent mice, and has not yet been documented.
The incidence of eosinophilic crystals is high in aging B6;129 mice, a hybrid background often encountered in studies using genetically engineered mice. It is observed in lungs (36% of males and 65% of females) and nasal turbinates (4% of males and 12% of females)4. The so-called eosinophilic crystalline pneumonia is a major cause of death in 129/SvJ mice and immunohistochemical studies show that crystals are composed predominantly of Ym1 protein, a chitinase-like protein known to be secreted by activated macrophages5. In our case, the context of chronic granulomatous inflammation with numerous activated macrophages is very likely the direct cause of Ym1 protein accumulation and crystallization.
JPC Diagnosis: Subcutis: Cellulitis, pyogranulomatous, focally extensive, severe with numerous colonies of cocci, Splendore-Hoeppli material, with mild to moderate granulomatous lymphadenitis and sialoadenitis.
Conference Comment: Botryomycosis is a chronic pyogranulomatous disease which is as well known in mice as it is poorly named. This inflammatory lesion is seen in a wide range of mammals including man, mice, dogs, cattle6, swine, apes, and elephants, and likely many other in species. The lesion, which consists of colonies of bacteria surrounded by aggregates of antigen-antibody complexes (known as Splendore-Hoeppli material), goes also by the name of “bacterial pseudomycetoma”, “bacterial pseudomycosis”, “bacterial granuloma”, and “granulomatosis”. It has no connection to fungal infections, other than a passing resemblance to mycetomas, or deep fungal infections which are characterized by “grains”.
Historically, the first cases of botryomycosis were observed in the late 1800s in post-surgical cattle and horses, with the first actual description of botryomycosis in a horse in 1870 by Bollinger. The first human case of botryomycosis was not reported until 1913. The causality of Staphylococcus aureus and description of Splendore-Hoeppli phenomenon was first made in 1919.4
Botryomycosis is an uncommon disease in humans with approximately 200 cases reported to date. Case distribution is worldwide, and the disease predominates 2:1 men with no age predilection. 75% of reported cases are cutaneous, with the rest visceral. Accidental or postoperative skin trauma and altered immune function are considered major contributing factors.4
The pathogenesis of botryomycosis in humans and animals has not been explicitly defined, but several factors appear to be necessary. Most causative microorganisms are of low virulence. The contributor lists the commonly implicated organisms (above). Implicated anaerobes include Propionibacterium acnes and Bacteroides species. Rare causes include Actinobacillus lignieresi, Serratia marcescens, Pneumocystis jirovecii, and Moraxella sp4.
A wide range of immune dysfunctions have been associated with the development of botryomycosis in humans and animals.4 It has been found more often in animals with deficient cellular immune responses including lymphopenia (nude mice) and various hypoglobulinemic syndromes (agammaglobulinemic mice).
Cutaneous botryomycosis require skin trauma in most cases, as low-virulence bacteria are generally unable to cross an intact barrier. The inoculum of bacteria must be high enough to evade the body’s immediate immune response, yet low enough not to cause massive necrosis or systemic disease. In all but severely immunosuppressed patients, the Splendore-Hoeppli phenomenon (SHP) is present. SHP assists in clustering the bacteria to create a stage of resistance. The major component of SHP is antigen-antibody complexes, but other substances are often present, to include immunoglobulin G, C3 fragments of complement, fibrin, and cellular debris.4
Both cutaneous and visceral forms of botryomycosis are well documented in man in animals. In humans, cutaneous forms most often affect expose parts of the body including the hands, feet, head, and neck. Visceral forms may be seen in almost 10 organ and in humans often accompanies prolonged hospital stay’s, especially in immunosuppressed patients. The most frequent visceral organs involved or the lungs, and are often associated with patient suffering from cystic fibrosis. HIV/AIDS is also a common predisposing condition.4
Contributing Institution:
Department of Pathology, Nantes-Atlantic National College of Veterinary Medicine, Food Science and Engineering - ONIRIS, 44 307 Nantes Cedex 03, France.
www.oniris-nantes.fr
References:
1.Bridgeford EC, Fox JG, Nambiar PR, Rogers A B. Agammaglobulinemia and Staphylococcus aureus botryomycosis in a cohort of related sentinel Swiss Webster mice. J Clin Microbiol 2006, 46, 1881–1884.
- Haines DC, Chattopadhyay S, Ward, JM. Pathology of aging B6;129 mice. Toxicol Pathol 2001; 29: 653–661 (2001).
- Hoenerhoff MJ, Starost MF, Ward JM. Eosinophilic crystalline pneumonia as a major cause of death in 129S4/SvJae mice. Vet Pathol 2006; 43, 682-688.
- Padilla-Desgarennes C, Vázquez-González D., Bonifaz A. Botryomycosis. Clin Dermatol 2012; 30, 397–402.
- Percy DH, Barthold SW. Mouse. In Pathology of Laboratory Rodents and Rabbits 73–76 (2007).
- Spagnoli S, Reilly TJ, Calcutt MJ, Fales WH, Kim DY. Subcutaneous botryomycosis due to Bibersteinia trehalosi in a Texas longhorn steer. Vet Pathol 49(5):775-778.