Signalment:
Gross Description:
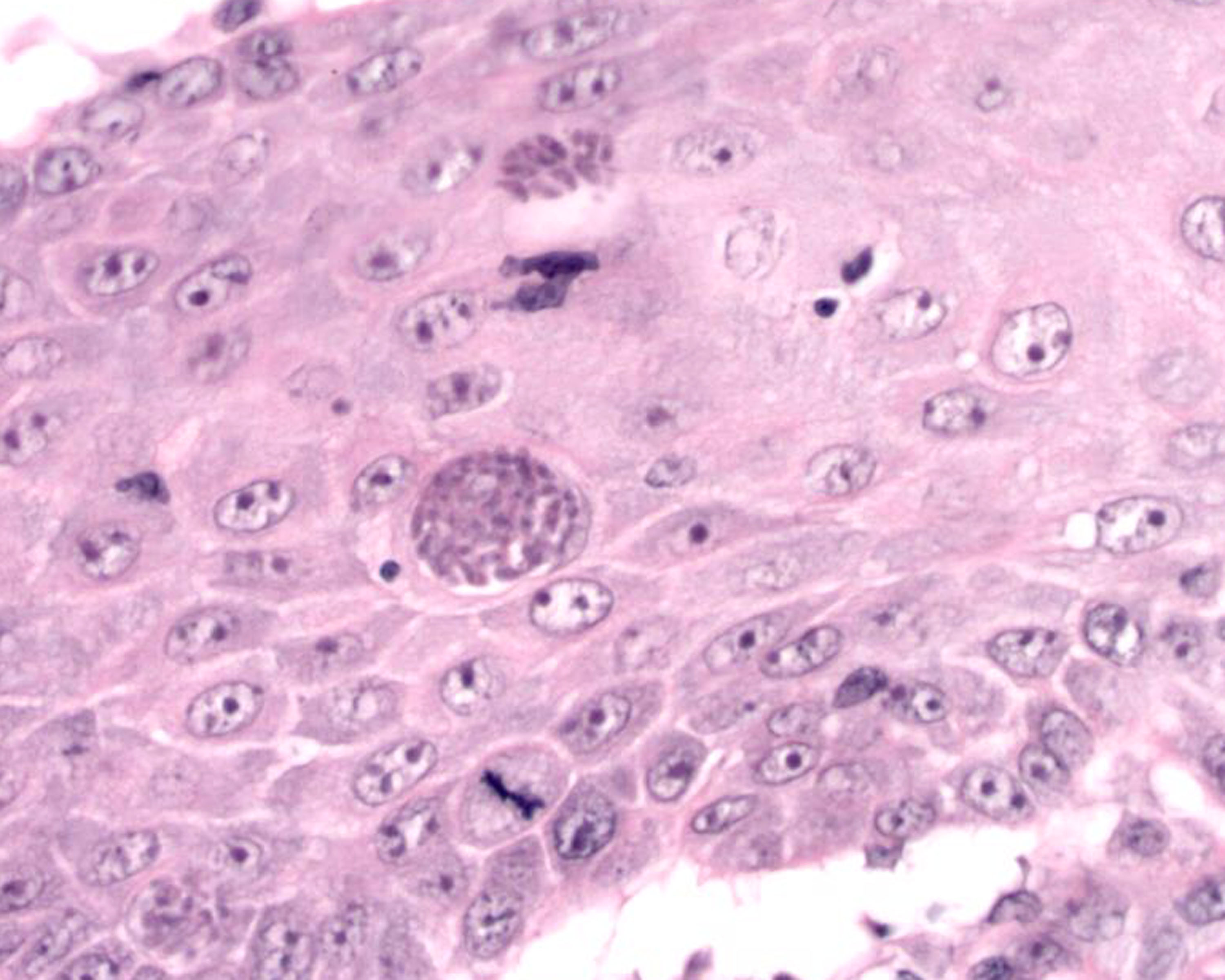
Histopathologic Description:
Morphologic Diagnosis:
2. Moderate to marked, diffuse, interstitial pyogranulomatous dermatitis with intrahistiocytic, intraendothelial and free protozoal zoites: DDx: Neospora
3. Moderate to marked, multifocal, neutrophilic folliculitis and pyogranulomatous furunculosis with numerous intrakeratinocyte and free protozoal zoites:DDx Neospora
Lab Results:
Anti-Toxoplasma IgM Indirect Immunofluorescence (IFAT) < 1:32
Anti-Neospora Indirect Immunofluorescence (IFAT) > 1:25600
Indirect Immunohistochemistry: Anti-Neospora Antibody (monoclonal): positive;
Anti-Toxoplasma Antibody (polyclonal).Â
Microbiology: Negative for fungal and bacterial growth
The two samples from the skin of the dog were strongly positive for Neospora caninum with a Neospora qPCR and a nested Neospora PCR.
Condition:
Contributor Comment:
Cutaneous Neosporosis has been reported in dogs before, although it is more commonly recognized as a cause of neuromuscular disease in young dogs and abortion in cattle2. The predominately cutaneous manifestation of Neosporosis demonstrated in this case may be associated with the concurrent immunotherapy this dog was receiving. CD4+ T-cells have been shown to play an important role in mice in protecting them against N. caninum infection8. Although cyclosporine is recognized to be an effective treatment for canine atopy with minimal side effects9, the combination of prednisolone and cyclosporine treatment in this dog would have had a suppressive effect upon cell mediated immunity which is important in protecting dogs against N. caninum infection8. Neosporosis has been previously reported in an adult dog receiving prednisone and azathioprine6.Â
JPC Diagnosis:
Conference Comment:
Neosporosis affects a variety of species including sheep, goats, and deer, but most importantly, dogs and cattle.4 It is reported to be one of the most important causes of bovine abortion, and transplacental transmission can occur.4 In dogs, neurological disease in puppies is common, and cutaneous manifestations have been reported in immunosuppressed animals.4 Histologically, cutaneous lesions are composed of pyogranulomatous and eosinophilic to necrotizing and hemorrhagic dermatitis.7 Diagnosis primarily relies on serologic testing.7
N. caninum can be distinguished from T. gondii based on the following ultrastructural features.1
| Neospora caninum | Over 11 rhoptries Tachyzoites often not within a parasitophorous vacuole Tissue cysts are relatively uncommon |
| Toxoplasma gondii | Few rhoptries Always found in membrane-bound vacuole in cytoplasm |
We thank Dr. C. H. Gardiner, PhD, veterinary parasitology consultant to the AFIP, for his review of this case.
References:
2. Dubey JP: Review of Neospora caninum and neosporosis in animals. Korean J Parasitol 41:1-16, 2003
3. Gardiner CH, Fayer R, Dubey JP: An Atlas of Protozoan Parasites in Animal Tissues, 2nd ed., pp. 59-60. Armed Forces Institute of Pathology, Washington, DC, 1998
4. Ginn PE, Mansell JEKL, Rakich PM: Skin and appendages. In: Jubb, Kennedy and Palmers Pathology of Domestic Animals, ed. Maxie MG, 5th ed., vol. 1, p. 711. Elsevier Saunders, Philadelphia, PA, 2007
5. Maie MG, Youssef S: Nervous system. In: Jubb, Kennedy and Palmers Pathology of Domestic Animals, ed. Maxie MG, 5th ed., vol. 1, pp. 436-437. Elsevier Saunders, Philadelphia, PA, 2007
6. Ordeix L, Lloret A, Fondevila D, Dubey JP, Ferrer L, Fondati A: Cutaneous neosporosis during treatment of pemphigus foliaceus in a dog. J Am Anim Hosp Assoc 38:415-419, 2002
7. Scott DW, Miller WH, Griffin CE: Viral, rickettsial, and protozoal skin diseases. In: Muller and Kirks Small Animal Dermatology, 6th ed., pp. 532-533. Saunders, Philadelphia, PN, 2001
8. Steffan J, Favrot C, Mueller R: A systematic review and meta-analysis of the efficacy and safety of cyclosporin for the treatment of atopic dermatitis in dogs. Vet Dermatol 17:3-16, 2006
9. Tanaka T, Hamada T, Inoue N, Nagasawa H, Fujisaki K, Suzuki N, Mikami T: The role of CD4+ or CD8+ T cells in the protective immune response of BALB/c mice to Neospora caninum infection. Vet Parasitol 90:183-191, 2000