CASE I: 16855 (JPC 4157763)
Signalment:
2-year-old, female, Montana Tropical, Bos taurus, bovine.
History:
Two of 341 animals presented for swelling of the nose and lips (hippo face) and chest edema. These animals were being fed in native field.
Gross Pathology:
Inspection of the carcass revealed that no other organs except the head were involved.
Grossly, on the dorsal surface of tongue shaft raised firm nodules and plaques, between 0.5 to 2 cm in diameter. Soft tissues of mandible, especially pharyngo-laryngeal lymph nodes, salivary glands, lips, nostrils and tonsils were swollen and contained whitish nodules when incised.
Laboratory Results:
Actinobacillus lignieresii was cultured.
Microscopic Description:
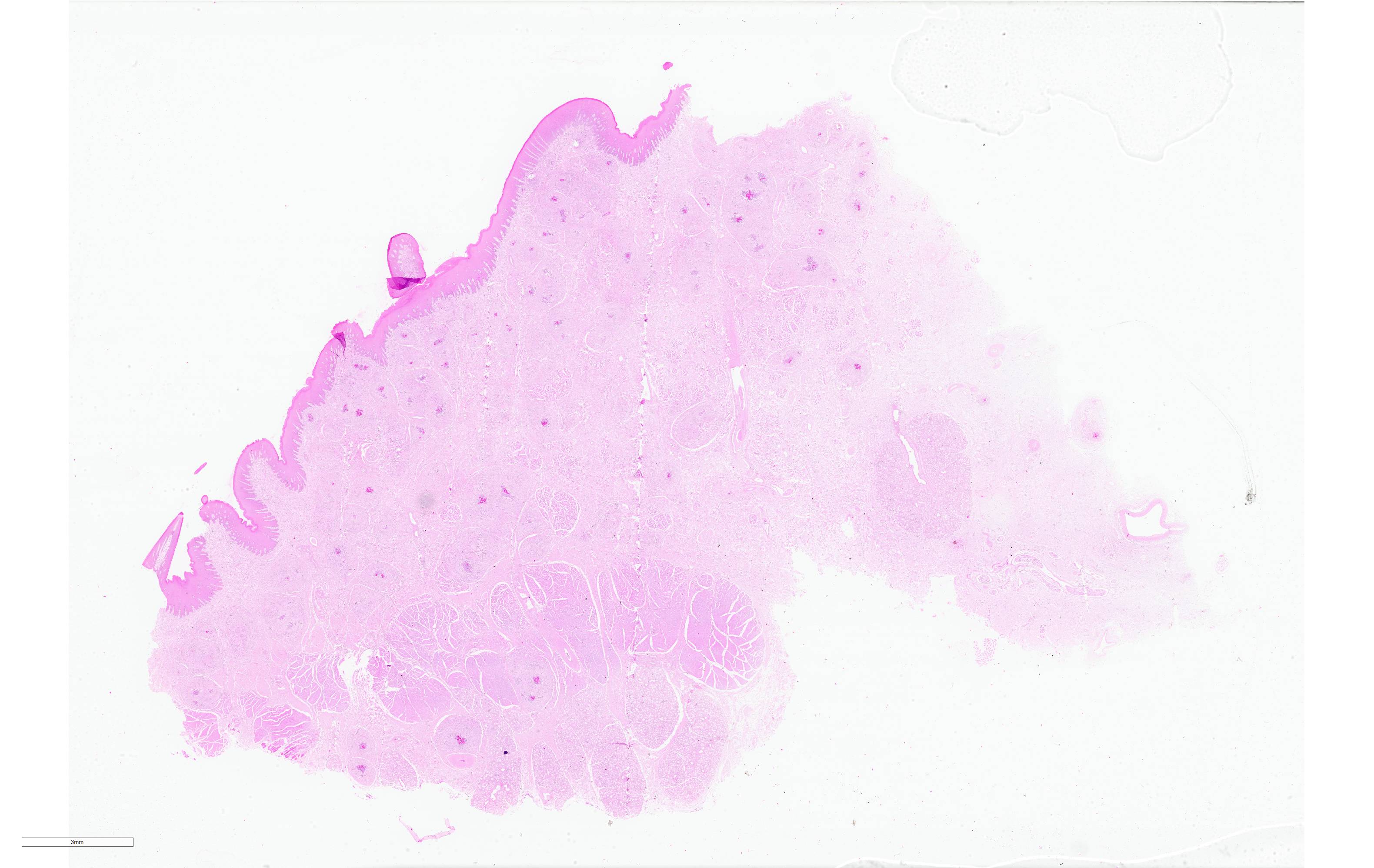
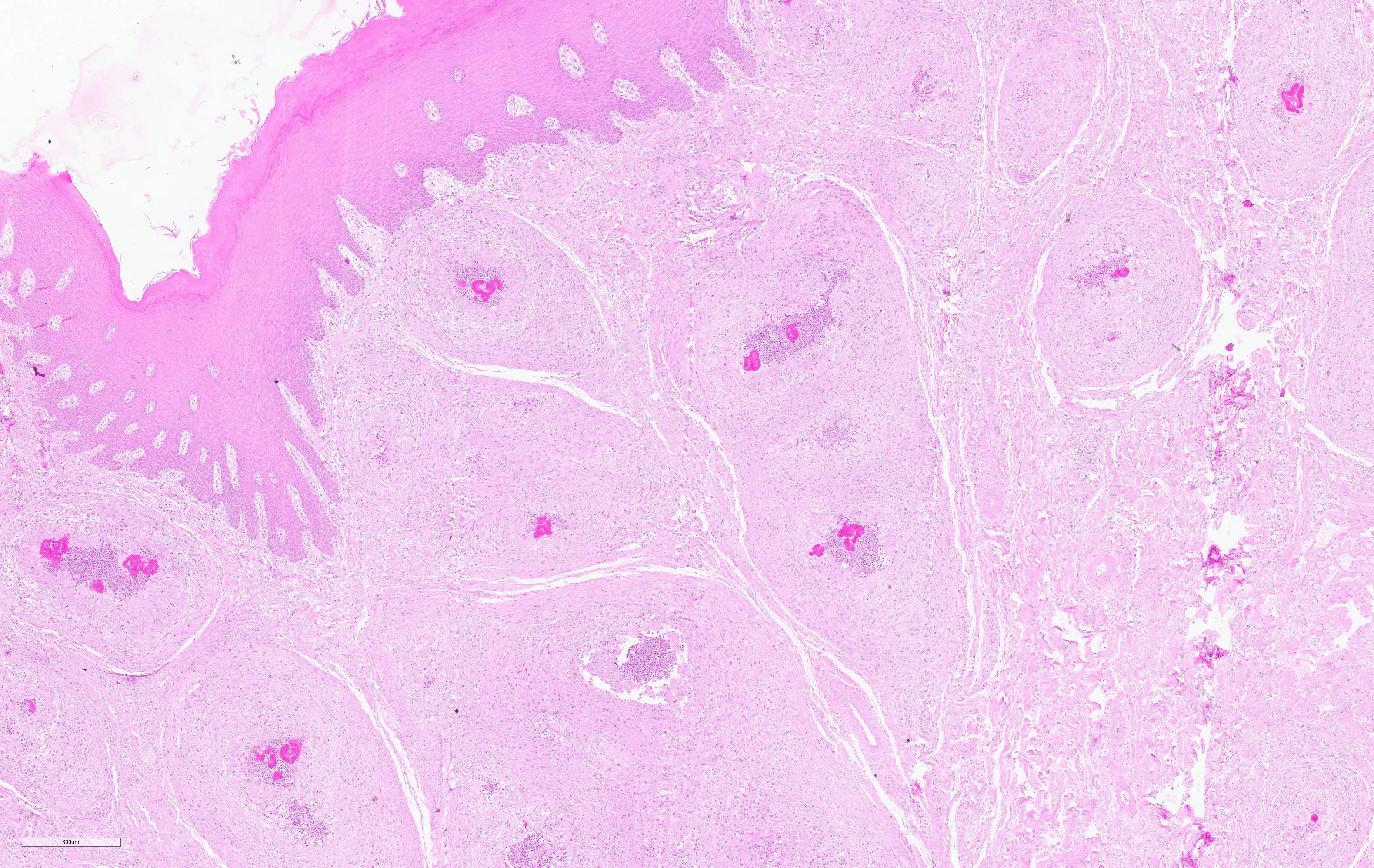
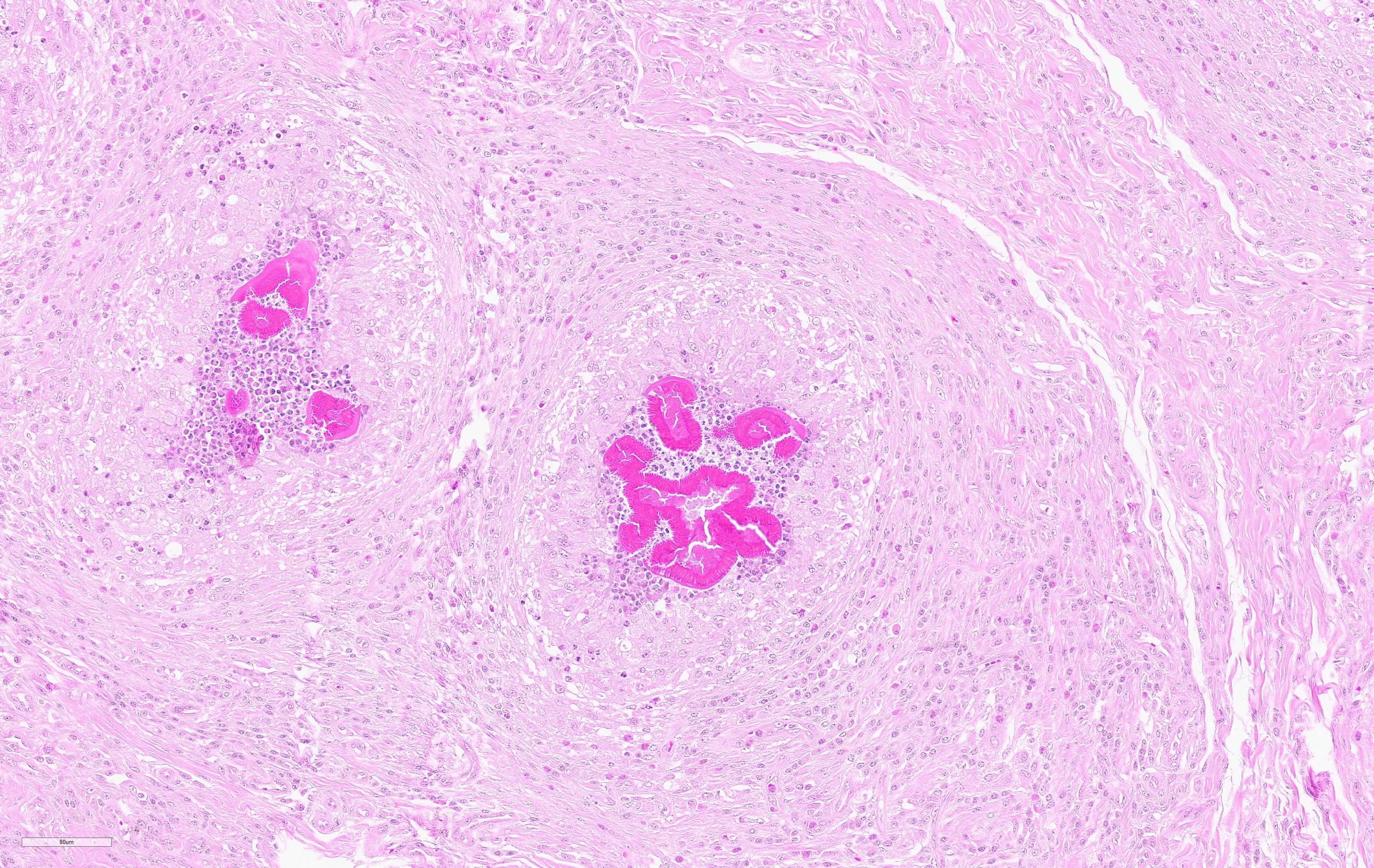
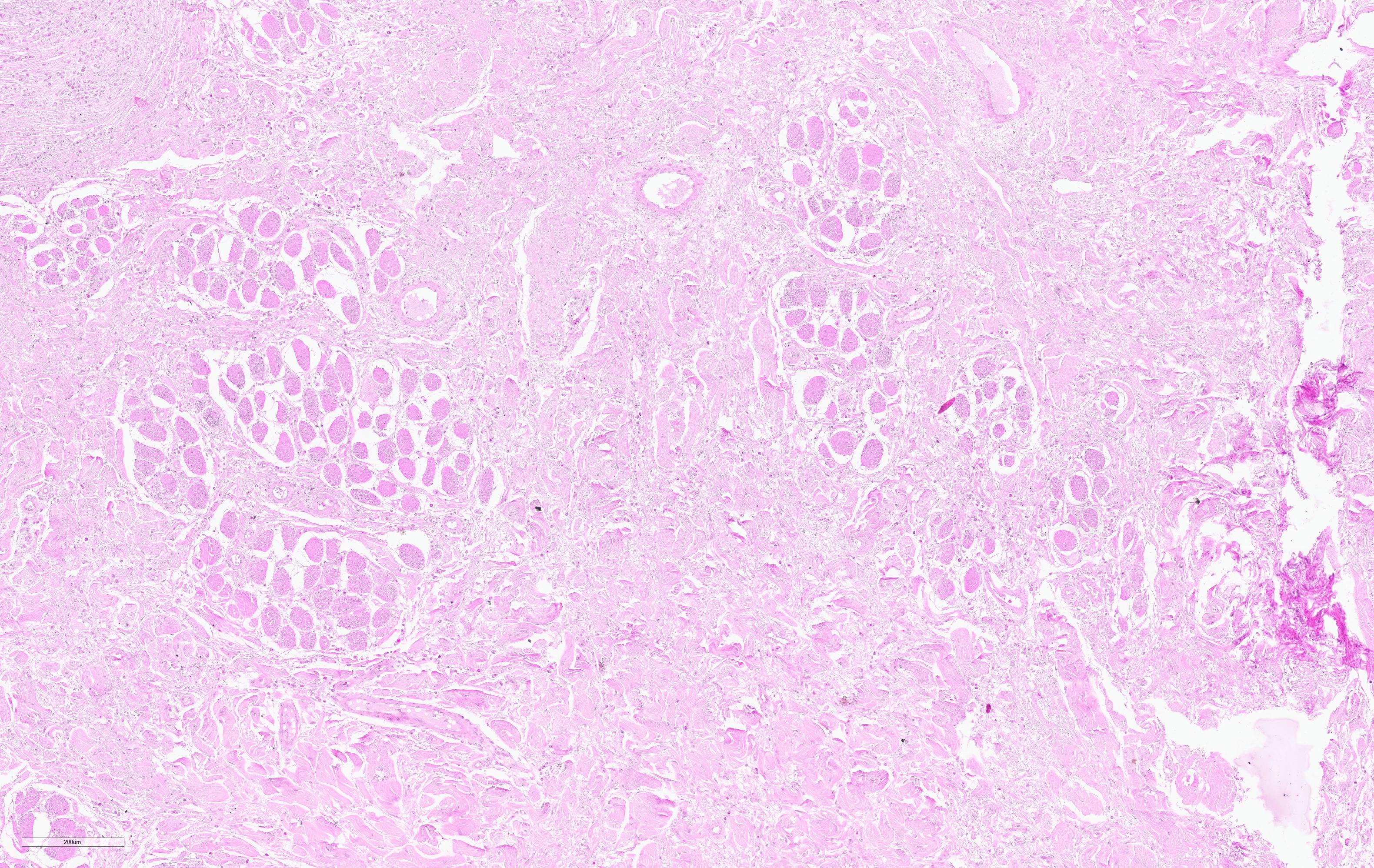
Histopathological examination of the skin and nasal soft tissues showed a thickened epidermis with scarring of the dermis and multiple pyogranulomas in the deep dermis. Within the lesions there were macrophages, epithelioid and multinucleated inflammatory giant cell and distinct rosettes of slender clubs with Gram-negative coccobacilli organisms at their center.
Contributor's Morphologic Diagnosis:
Rhinitis pyogranulomatous, bovine.
Contributor's Comment:
Actinobacillosis is a sporadic infectious animal disease caused by the Gram-negative bacilli Actinobacillus lignieresii. It is a common commensal inhabitant of the ruminant oral cavity. The bacteria can cause infection by invading adjacent soft tissues after the development of a penetrating wound.4
The genus Actinobacillus has remained relatively obscure until recently. In part, this must be due to there having been no recognized medical pathogen in the group to provoke research interest. The type species, A. lignieresii, has been recognized for many years as the cause of actinobacillosis in cattle and sheep. Latterly, the group has been growing with the recognition of A. actinomycetemcomitans as a significant cause of periodontal disease and the transfer from Haemophilus of A. pleuropneumoniae, an economically significant cause of respiratory disease in the pig. Through intense research interest focused on these two species, a much improved understanding of the bacteria has been acquired.8
The infection is characterized as a pyogranulomatous inflammation of the tongue, but also soft tissues as lymph nodes, other digestive tract localization and skin.6 In our case, the inflammation spreads to the lips, palate, nostrils and nasal cavity. Because of that, the animal face assumed the aspect called ?hippopotamus face?.
Contributing Institution:
Regional Diagnostic Laboratory, Veterinary Faculty
Federal University of Pelotas. 96010-900 Pelotas, RS, Brazil.
https://wp.ufpel.edu.br/lrd/
JPC Diagnosis:
Nasal/oral mucosa: Pyogranulomas, multifocal to coalescing, with Splendore-Hoeppli material.
JPC Comment:
Actinobacillus lignieresii was first identified as a pathogen by Lignierès and Spitz in South America during the early 20th century. A member of the family Pasteurellaceae, A. lignieressii is a commensal inhabitant of the upper digestive tract of ruminants and sporadically causes disease in cattle, sheep, goats, and rarely in other species. The condition is commonly associated with coarse poor-quality feed which is thought to cause traumatic inoculation; however other potential predisposing factors may include oral lesions secondary to viral infection, stress, and immunosuppression.1
In cattle, sheep, and goats, pyogranulomas caused by A. lignieresii most commonly occur in the soft tissues of the head and oral cavity and less often in other locations such as the forestomaches, lungs, and skin. Tongue lesions occur most often in cattle, commonly at the lingual groove, whereas sheep tend to develop lesions in the cutaneous and soft tissues of the lips and cheeks.3 This is likely due to differences in food prehension between species, with cattle primarily using the tongue whereas small ruminants predominantly utilize the lips. Regardless of species, the lesion is characterized by chronic pyogranulomatous inflammation with marked fibrosis resulting in progressive interference of prehension and mastication of feed, eventually resulting in loss of condition and may ultimately result in starvation.3 When the tongue is involved, it often becomes enlarged, firm, immobile, and may protrude from the mouth, resulting in the term "wooden tongue". Involvement of other organs, generally the skin or lymph nodes has been regarded as "atypical" or cutaneous actinobacillosis.3 Draining lymph nodes, including the parotid, submandibular, and reropharyngeal lymph nodes may be involved, resulting in regional lymphadenitis. Severe cases may result in esophageal and airway compression, potentially resulting in dyspnea and/or ruminal tympany.3
On cut surface, pyogranulomas are grossly visible as small, soft yellow or orange masses that often contain "sulfur" granules.1 Histologically, these granules correspond "club colonies" composed of gram negative coccobacilli surrounded by dense radiating eosinophilic club shaped Splendore-Hoeppli material. Club colonies are then surrounded by neutrophils, macrophages, and multinucleated giant cells. The surrounding reactive fibrous stroma and/or granulation tissue is further expanded by lymphocytes and plasma cells.10
Upon examination of previously described gross lesions, Actinomyces bovis should be considered as a leading differential diagnosis, although Nocardia sp., and tuberculosis should also be considered. A. bovis is a gram positive, non-acid fast filamentous bacterium that frequently forms sulfur granules. Although this pathogen is typically associated with chronic osteomyelitis ("lumpy jaw" or actinomycosis), it may involve soft tissues.1 Nocardia sp. is also a gram positive filamentous bacteria, but in contrast to A. bovis, Nocardia sp. are variably acid-fast and not typically associated with formation of sulfur granules. In Argentina, 14% of the lesions diagnosed macroscopically as tuberculosis by meat inspectors at slaughterhouses were actually actinobacillosis or actinomycosis. Therefore, actinobacillosis should be considered as differential in the diagnosis of tuberculosis and the importance of pursuing histologic and microbiologic examinations of compatible gross lesions for pathologic and etiologic confirmation.1
The moderator discussed use of the mnemonic "YAACSS-NT" (or "SSTAACY-N") as a memory aid when developing a differential diagnosis for genera commonly associated with the formation of large colonies. These genera include Yersinia, Actinomyces, Actinobacillus, Corynebacterium, Streptococcus, Staphylococcus, Trueperella, and occasionally Nocardia. It is important to state this list is not all-inclusive and other genera may also form colonies.
Many participants were unaware of the term "hippo face", a term which has been used in a scientific paper to describe the clinical manifestation of diffuse lesions affecting on the lips, palate, pharynx, nasal pits and face, which result in a unique "hippopatamous-like" appearance, much in the same manner as "wooden tongue".10 A similar lesion caused by Mannheimia granulomatis has been described affecting the muzzles of white-tailed deer and mule deer.5
References:
1. Caffarena RD, Rabaza A, Casaux L, et al. Natural lymphatic ("atypical") actinobacillosis in cattle caused by Actinobacillus lignieresii. J Vet Diagn Invest. 2018;40(2):218-225.
2. Fenwick BW, Woolums AR. Pasteurellaceae: Actinobacillus. In: McVey DS, Kennedy M, Chenappa MM, eds. Veterinary Microbiology, 3rd Ed. Ames, IA: John Wiley and Sons. 2013:108-114.
3. Henton MM, Van Der Lugt JJ. Acintobacillus ignieresii infections. In: Coetzer JAW, Tustin RC, eds. Infectious Diseases of Livestock, 2nd Ed. Cape Town, South Africa: Oxford University Press Southern Africa. 2004:1648-1650.
4. Kasuya K, Manchanayake T, Uenoyama K, et al. Multifocal suppurative granuloma caused by Actinobacillus lignieresii in the peritoneum of a beef steer. J Vet Med Sci. 2017;79(1):65-67.
5. Keel MK, Keeler S, Brown J, et al. Granulomatous Inflammation of the Muzzle in White-Tailed Deer (Odocoileus virginianus) and Mule Deer (Odocoileus hemionus) Associated With Mannheimia granulomatis. Vet Pathol. 2020;57(6):838-844.
6. Margineda CA, Odriozola E, Moreira AR et al. Atypical actinobacillosis in bulls in Argentina: granulomatous dermatitis and lymphadenitis. Pesq Vet Bras. 2014;44(1):1-5.
7. Relun A, Cesbron N, Bourdeau P, et al. Atypical actinobacillosis affecting hind limbs and lungs in a single beef cattle herd. J Vet Intern Med. 2019;44(1):297-401.
8. Rycroft AN, Garside LH. Actinobacillus species and their role in animal disease. Vet J. 2000;159(1):18-46.
9. Scheid HV, Estima-Silva P, Monteiro FL, et al. Actinobacillosis outbreak in cattle with clinical manifestation of hippopotamus-like face. Pesq Vet Bras. 2020;40(5):355-359.
10. Uzal F, Plattner BL, Hostetter JM. Alimentary system. In: Maxie MG, ed. Jubb, Kennedy, and Palmer's Pathology of Domestic Animals, 6th ed. St' Louis, Missouri: Elsevier; 2016: Vol 2: 18-19.