Signalment:
Gross Description:
Other lesions included slight petechial hemorrhages of the stomach mucosa (confirmed by histology and associated with a laminar marked endothelial mineralization and necrosis on Alizarin red stain). Spleen was mildly firm, increased in size, and liver slightly and diffusely dark (HE and Perls stained slides: splenic and hepatic hemosiderosis and splenic macrophagous hyperplasia and extramedullary hematopoe+â-»sis). 10 mL of serous pericardial effusion was found.
Histopathologic Description:
PAS staining: glomerular hypercellularity with both mesangial and endocapillary proliferation. Glomerular basement membranes are thickened.
Gomori Staining: multifocally, there are red dots in podocyte cytoplasm and basement membrane, and there are fibrotic glomerular and interstitial changes.
Morphologic Diagnosis:
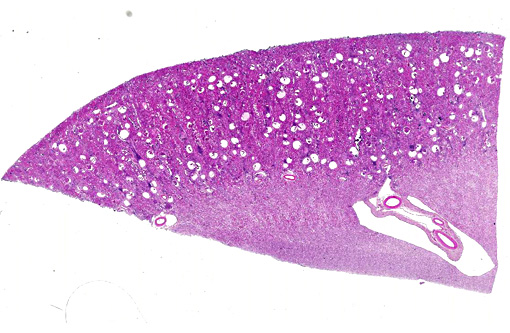
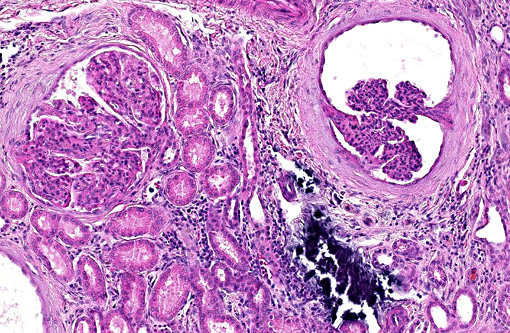
Kidney: glomerulonephritis, membranoproliferative, diffuse, marked, chronic, with proteinuria, glomerular microcysts and fibrotic changes.
Kidney: interstitial nephritis, lymphoplasmocytic and fibrotic, mild, multifocal, chronic.
Lab Results:
Condition:
Contributor Comment:
Defects in the glomerular selective filtration result in proteinuria and renal insufficiency, whose clinical spectra ranges from asymptomatic or proteinuric dogs, to non specific presentation (weight loss, apathy, anorexia), or evident signs of chronic renal insufficiency (polyuria, polydipsia, vomiting, halitosis).(6) Extrarenal complications of glomerular diseases include: nephrotic syndrome (hypoalbuminemia, proteinuria, hypercholesterolemia, edema, serous effusions); thromboembolism, secondary to loss of antithrombin III; hypertensive illnesses; and microangiopathic anemia.(2,6)
Glomerular diseases can be acquired or congenital. Acquired glomerular injuries can result from:
- Immune complex deposition (glomerulonephritis proliferative, membranous, membranoproliferative). Etiologies range from chronic infections (canine pyometra, Borrelia burgdoferi, etc.) to immune-mediated diseases (systemic erythematous lupus).(3)
- In situ Immune complex formation (anti-GBM glomerulonephritis). Antibodies bind on GBM antigens. It is rare in domestic animal, and suspected in several dogs. In humans, antibodies cross-reaction occurs by antigenic mimicry between streptococcus and GBM for instance.(3,6)
- Damage by systemic factors affecting the glomeruli. It includes mesangial deposits like amyloidosis, focal segmental glomerulosclerosis, and minimal change disease.(6)
Congenital glomerulopathy gathers an increasing number of breeds, whose pathogeny and mode of inheritance often remains unknown and varies a lot between breeds. The table lists dog breeds with reported familial glomerulopathies.(3)
| Breed | Glomerulopathy |
| Beagle | Amyloidosis Membranoproliferative glomerulonephritis |
| Bernese mountain dog | Membranoproliferative glomerulonephritis |
| Bull terrier | Hereditary nephritis |
| Bullmastiff | Focal and segmental glomerulosclerosis |
| English cocker spaniel | Hereditary nephritis |
| Dalmatian | Hereditary nephritis |
| Doberman pinscher | Glomerulosclerosis Cystic glomerular atrophy |
| English foxhound | Amyloidosis |
| French mastiff | Juvenile glomerulopathy |
| Greyhound | Glomerular vasculopathy and necrosis |
| Newfoundland | Glomerulosclerosis |
| Pemprobe Welsh corgi | Cystic glomerular atrophy |
| Rottweiler | Atrophic glomerulopathy |
| Samoyed | Hereditary nephritis |
| Shar-Pei | Amyloidosis |
| Soft-coated wheaten terrier | Proliferative and sclerosing glomerulonephritis |
In Bernese Mountain Dogs, a familial glomerulopathy was reported by Minkus and collaborators in 1994. Lesions included membranoproliferative glomerulonephritis, with concomitant interstitial nephritis and high titer of IgG against Borrelia burgdorferi.(4) Since then, few reports were published, but one of them highlights an absence of correlation between proteinuria, the early sign of glomerular lesions, and the antibodies against B.burgdoferi.(1)
The present case deals with a 2.5-year-old Bernese mountain dog with chronic renal insufficiency and histologic lesions compatible with membranoproliferative glomerulonephritis and interstitial nephritis; however, immunofluorescence should have been performed to confirm it. A proliferation of myoepithelial periglomerular artierioles was also suspected and supports a probable hypertensive state that has not been clinically evaluated.
JPC Diagnosis:
Conference Comment:
References:
1. Gerbe, B, Eichenberger S, Haug K, Wittenbrink MM, & Reusch CE (2009). Association of urine protein excretion and infection withBorrelia burgdorferisensu lato in Bernese Mountain dogs. Vet J, 182(3), 487-488.
2. Kumar V, Abbas AK, Fausto N, & Aster JC (2009). Robbins and Cotran Pathologic Basis of Disease, Professional Edition: Expert Consult-Online. Elsevier Health Sciences.
3. Maxie MG, Newman SJ. Urinary system. In : Maxie MG, ed. Jubb, Kennedy and Palmers Pathology of Domestic Animals. 5th ed. Vol. 2. Philadelphia, PA : Elsevier Saunders ; 2007 :459-461.
4. Minkus G, Breue, W, Wanke R, Reusch C, Leuterer G, Brem G, & Hermanns W (1994). Familial nephropathy in Bernese mountain dogs. Vet Pathol, 31(4), 421-428.
5. Newman SJ. The urinary system. In : Zachary JF, McGavin MD, eds. Pathologic Basis of Veterinary Disease. 5th ed. St. Louis, MO : Elsevier Mosby ; 2012 :620-627.
6. Vaden SL (2011). Glomerular disease. TopCompanion Anim Med, 26(3), 128-134.