Signalment:
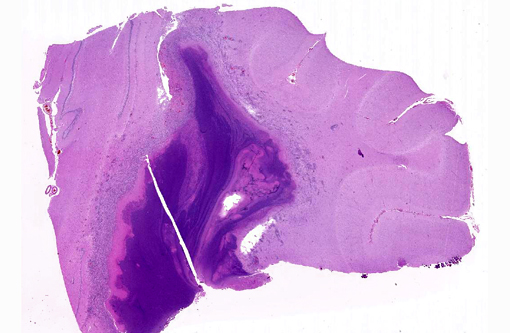
Gross Description:
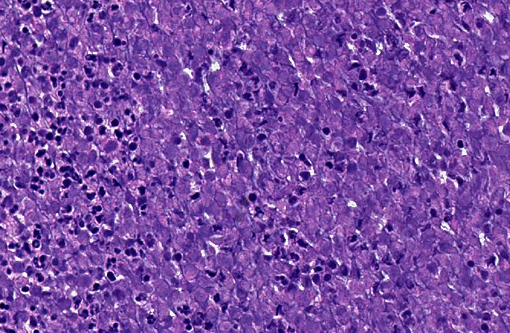
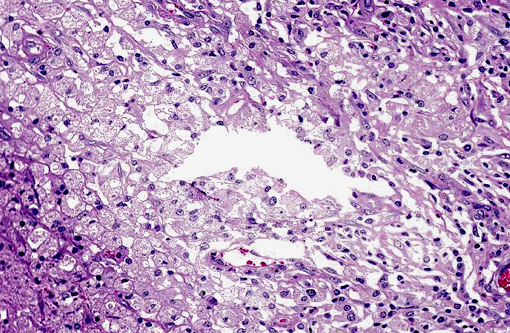
Histopathologic Description:
Morphologic Diagnosis:
Lab Results:
Condition:
Contributor Comment:
Certain buck behaviors, such as aggressive sparring and fighting, can cause damage to the antler pedicle and/or other parts of the skull that can predispose them to brain abscesses.(1)
Different studies, from 1996-2008, showed that the intracranial abscesses were diagnosed as the cause of death or illness in white-tailed deer examined by the diagnostic laboratories across portions of the United States and Canada. The bacterium Arcanobacterium pyogenes was the primary cause of infection.(1,2,3,5)
The clinical signs include several behavioral characteristics associated with the neurological system, such as circling or loss of coordination. Often times, deer can become emaciated, which is characterized by excessive weight loss or having a deteriorated appearance. Bucks also may have a puss-like substance located around the antler pedicle that leaks through openings in the skull. It is not known whether this disease can be transmitted between deer or other animals through direct contact or other sources. Also, it is important to note that deer with brain abscesses are not recommended for consumption.(1)
The clinical, gross examination and ancillary tests findings were compatible with the previous studies.
Note: Multiple blocks were used for the slides submission; therefore, not all the participants will get the same copy of the slides.
JPC Diagnosis:
Conference Comment:
For a deer exhibiting neurologic symptoms, the differential of Listeria monocytogenes must also be considered. Lesions of listeriosis are typically smaller (microabscesses) and confined to the brainstem.
There is an increasing trend for hunters and property owners to allow bucks to reach a more mature age before harvesting to improve herd health and antler quality.(1) Associated with the trend is the unintended consequence of increased numbers of brain abscesses occurring in mature males. Recently, a study of 26 collared bucks over 2.5 years old identified brain abscess as the cause of death in 35% of cases, likely related to the increased competition among mature bucks.(5)
Arcanobacterium progenies is the most commonly cultured isolate from brain abscess, being the only isolate in almost 50% of cases.(2) The bacterium has been through a series of name changes, and has recently been reclassified as Trueperella progenies based on DNA sequencing and mass spectrometry.(4)
References:
1. Basinger R. Brain Abscesses A potential thorn in the side of intensive deer management programs. Westervelt Wildlife Service. 2009;9:2631.
2. Baumann CD, Davidson WR, Roscoe DE, Beheler-Amass K. Intracranial abscessation in white-tailed deer of North America. J Wildl Dis. 2001;37(4):66170.
3. Hattel AL, Shaw DP, Love BC, Wagner DC, Drake TR, Brooks JW. A retrospective study of mortality in Pennsylvania captive white-tailed deer (Odocoileus virginianus): 20002003. J Vet Diagn Invest. 2004;16:515521.
4. Hijazin M, Hassan AA, Alber J, et al. Evaluation of matrix-associated laser desorption ionization-time of flight mass spectrometry (MALDI-TOF MS) for species identification of bacteria of genera Arcanobacterium and Trueperella. Vet Microbiol. 2012;157(1-2):243-245.
5. Karns GR, Lancia RA, Deperno CS, Conner MC, Stoskopf MK. Intracranial abscessation as a natural mortality factor for adult male white-tailed deer (Odocoileus virginianus) in Kent County, Maryland, USA. J Wildl Dis. 2009;45(1):196200.