Signalment:
Gross Description:
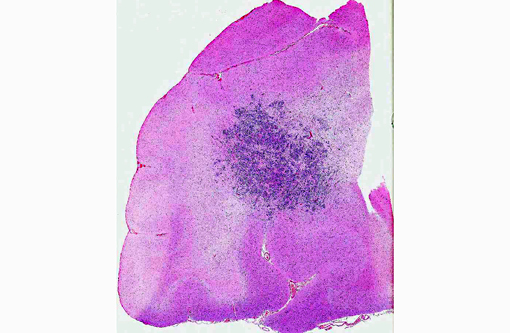
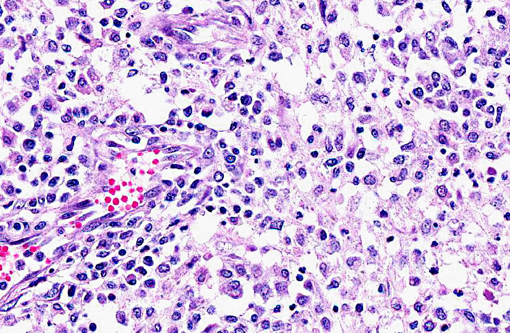
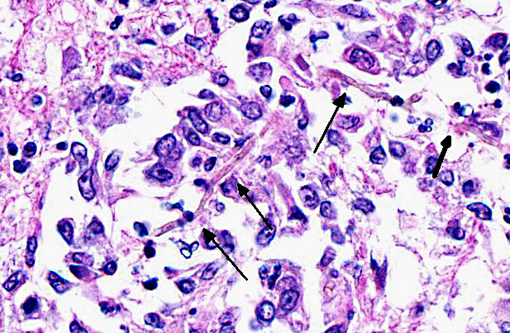
Histopathologic Description:
Morphologic Diagnosis:
Lab Results:
Complete blood count:
| Parameter | Result | Reference range |
| Nucleated cells | 2.9 x 103/μl | 4.5-15.0 x103/μl |
| Segmented neutrophils | 1.9x103/μl | 2.6-11.0x103/μl |
| Lymphocytes | 0.2x103/μl | 1.0-4.8x103/μl |
| Eosinophils | 0.1x103/μl | 0.1-1.2x103/μl |
| nRBCs | 0.1 x103/μl | 0.0x103/μl |
| RBC | 4.1x103/μl | 5.5-8.5x103/μl |
| HGB | 9.7 g/dl | 13.0-20.0 g/dl |
| PCV | 30.0% | 40.0-55.0% |
| MCV | 75.0 fl | 62.0-73.0 fl |
| MCHC | 32.0 g/dl | 33.0-36.0 g/dl |
| Reticulocytes | 85,050/μl | 0.0-60,000/μl |
Serum Chemistry:
| Parameter | Result | Reference range |
| Total protein | 7.3 gm/dl | 5.3-7.2 gm/dl |
| Globulin | 3.9 gm/dl | 2.0-3.8 gm/dl |
| ALP | 437 IU/l | 20-142 IU/l |
| ALT | 179 IU/l | 10-110 IU/l |
| GGT | 68 IU/l | 0-9 IU/l |
| Glucose | 534 mg/dl | 75.0-130.0 mg/dl |
| Anion gap | 26 | 13-22 |
Blood gas (venous):
| Parameter | Result | Reference range |
| pH | 7.119 | 7.3-7.5 |
| pCO2 | 40.3 mmHG | 24.0-39.0 mmHG |
| pO2 | 166.0 mmHG | 67.0-92.0 mmHG |
| HCO3 | 12.5 mm/L | 15.0-24.0 mm/L |
| Anion gap | 24 mEq/l | 13.0-22.0 mEq/l |
Condition:
Contributor Comment:
The various fungal species are not morphologically distinct on routine H&E histologic examination.(4) Culture, fungal morphology or molecular techniques are generally required for speciation.(6) Organisms in general have a dark brown to light yellow pigment, although degree of pigmentation can vary, and have 2-6 μm in width septate hyphae that can be branched or unbranched.(4,7) If melanin pigment is not identifiable, Fontana-Masson histochemical stain may assist in identification of subtle pigment.(4,7)
Phaeohyphomycotic fungi are composed of more than 100 different dematiaceous species presenting clinically as cutaneous, central nervous system and disseminated infections.(6,14,16) Reported most frequently in cats, phaeohyphomycosis has been occasionally documented in horses, dogs, cattle and goats.(5,7,12,15) Typically feline infections are limited to subcutaneous tissues although disseminated and cerebral forms do occur and are most often associated with immunologic compromise.(14,16) Cutaneous forms are thought to occur due to introduction of the organism via a penetrating wound.(14,16) Specifically, Cladophialophora bantiana, (also known as Cladosporium bantianum, Cladosporium trichoides, and Xylohypha bantiana) has a tropism for nervous tissue and has been reported as a cause for cerebral phaeohyphomycosis in both dogs and cats.(11,12)
Immunosuppression likely contributed to the pathogenesis of cerebral phaeohyphomycosis in this dog with a history of cyclosporine and prednisone administration for treatment of IMHA. Route of infection was unclear at the time of necropsy although ultimately hematogenous dissemination was suspected due to the presence of fungal organisms within the liver.
Cutaneous infection may have been the route of entry although lesions were absent at necropsy examination. Ingestion of the fungus and entry via the compromised stomach was considered but unlikely due the absence of histologic identification of the organism within sections of the stomach at the location and distant to the perforation.
JPC Diagnosis:
Conference Comment:
As noted in the summary, immunosuppression secondary to repeated administration of cyclosporine and prednisone for treatment of immune mediated hemolytic anemia likely predisposed this dog to fungal infection. With that in mind, conference participants briefly discussed the clinical pathologic findings in this case, which were consistent with the history of treatment for IMHA and the diagnosis of disseminated phaeohyphomycosis. Macrocytic, hypochromic, regenerative anemia is an expected finding in dogs with IMHA.(10) Corticosteroid treatment typically induces lymphopenia, and while neutrophilia is a common finding in cases of hemolysis and corticosteroid administration, the neutropenia observed in this case probably occurred due to the disseminated fungal infection.(10) Globulin concentration also increases in infection and inflammation.(10) Anemia induced hypoxic injury to centrilobular hepatocytes may result in elevation of ALT, while increased ALP and GGT may occur following corticosteroidinduced hepatocellular glycogen accumulation.(10) Corticosteroids also induce hyperglycemia.(10)
References:
2. Fothergill AW. Identification of dematiaceous fungi and their role in human disease. Clinical Infectious Diseases. 1996;22(8uppl 2): 8179-8184.
3. Frank C, Vemulapalli R, Lin T. Cerebral phaeohyphomycosis due to Cladophialophora bantiana in a Huacaya alpaca (Vicugna pacos). J Comp Pathol. 2011;145(4):410-413.
4. Ginn PE, Mansell JEKL, Rakich PM. Skin and appendages. In: Maxie MG, ed. Jubb, Kennedy and Palmers Pathology of Domestic Animals. 5th ed. Vol. 1. Philadelphia, PA: Elsevier Inc; 2007:702-703.
5. Giri DK, Sims WP, Sura R, Cooper JJ, Gavrilov BK, et al. Cerebral and renal phaeohyphomycosis in a dog infected with Bipolaris species. Vet Pathol. 2011;48:754-757.
6. Grooters AM, Foil CS. Miscellaneous Fungal Infections. In: Greene CE ed. Infectious Disease of the Dog and Cat. 3rd ed. Elsevier Inc; 2006:647-649.
7. Herra-�ez P, Rees C, Dunstan R. Invasive phaeohyphomycosis caused by Curvularia species in a dog. Vet Pathol. 2001;38:456459.
8. Janovsky M, Grone A, Ciardo D, Vollm J, Burnens A, Fatzer R, et al. Phaeohyphomycosis in a snow leopard (Uncia uncia) due to Cladophialophora bantiana. J Comp Pathol. 2006;134(2-3):245-248.
9. Langfelder K, Streibel M, Jahn B, Haase G, Brakhage AA. Biosynthesis of fungal melanins and their importance for human pathogenic fungi. Fungal Genetics and Biology. 2003;38:143158.
10. Latimer KS, ed. Duncan and Prasses Veterinary Laboratory Medicine Clinical Pathology. 5th ed. Ames, IA: John Wiley and Sons; 2011:65,178-179,386-388.
11. Lavely J, Lipsitz D. Fungal infections of the central nervous system in the dog and cat. Clin Tech Small Anim Pract. 2005;20:212-219.
12. Migaki G, Casey HW, Bayles WB. Cerebral phaeohyphomycosis in a dog. J Am Vet Med Assoc. 1987;191: 997-998.
13. Olias P, Hammer M, Klopfleisch R. Cerebral phaeohyphomycosis in a green iguana (Iguana iguana). J Comp Pathol. 2010;143(1):61-64.
14. Revankar SG, Patterson JE, Sutton DA, Pullen R, Rinaldi MG. Disseminated Phaeohyphomycosis: Review of an emerging mycosis. Clinical Infectious Diseases. 2006;34:467476.
15. Singh K, Flood J, Welsh RD, Wickoff III JH, Snider TA, Sutton DA. Fatal systemic phaeohyphomycosis caused by Ochroconis gallopavum in a dog (Canis familaris). Vet Pathol. 2006;43:988992.
16. Swift, IM, Griffin A, Shipstone MA. Successful treatment of disseminated cutaneous phaeohyphomycosis in a dog. Australian Veterinary Journal. 2006;84:431-435.