Joint Pathology Center
Veterinary Pathology Services
Wednesday Slide Conference
2019-2020
Conference 24
29 April, 2020
CASE III: S1706449 (JPC 4117527). Tissue from a horse (Equus caballus).
Signalment: Two-year-old Quarter horse gelding
History: Colic of unknown duration which could not be controlled with non-steroidal anti-inflammatory drugs (banamine and others) and was euthanized.
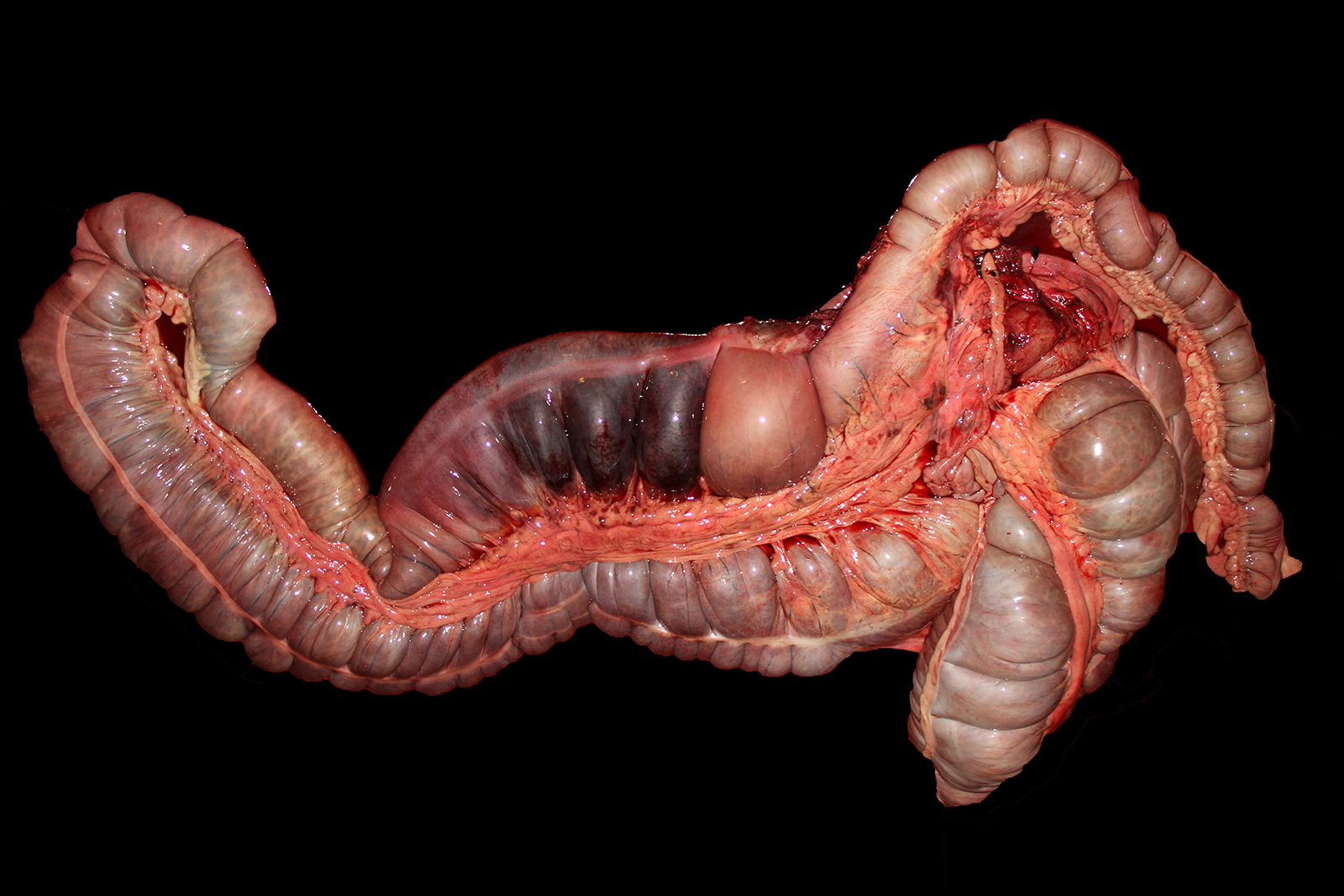
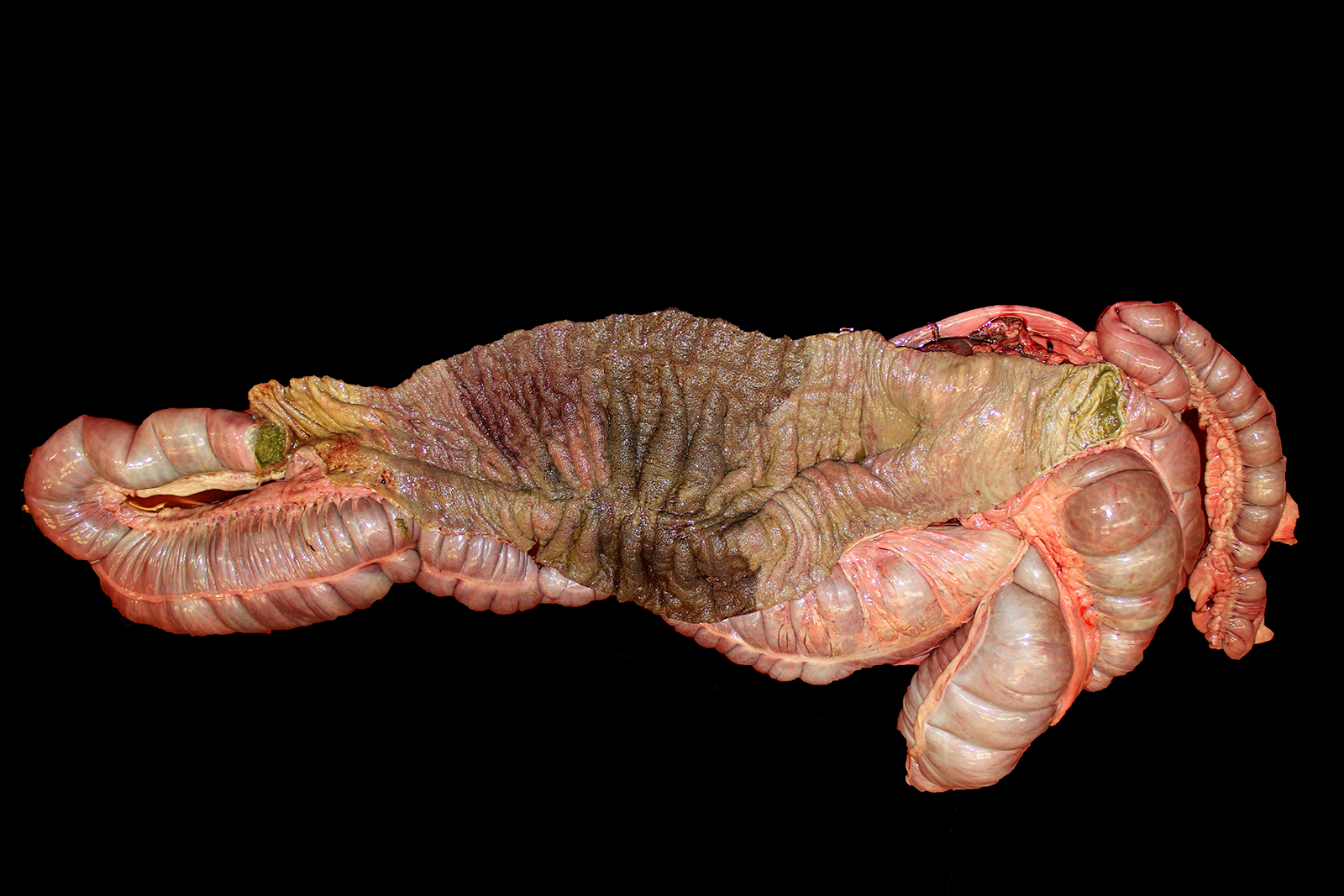
Gross Pathology: The carcass was in good nutritional condition, well-muscled and with adequate subcutaneous, peri-renal and pericardial adipose tissue. The abdomen contained approximately 1 liter of red, thin, opaque fluid. Affecting three quarters of the right dorsal colon, extending distally from the diaphragmatic flexure, were the following changes: the serosa was diffusely red to dark red; the wall was transmurally thickened up to 2 cm and dark red and wet; the mucosa was mottled red to dark red to brown with a diffusely corrugated appearance; and the ingesta was semi-liquid green plant material that was red-tinged. There was a sharp line of demarcation between this region and the distal one quarter of the right dorsal colon, which had a slightly less thickened wall and diffusely tan serosa and mucosa (Figs. 1 and 2). There was extensive petechiation of the epicardial surfaces of the atria and ventricles of the heart. No other significant gross abnormalities were observed in the rest of the carcass.
Laboratory results: Aerobic and anaerobic culture of colon tissue and content grew large mixed flora; culture of colon content for Clostridium difficile was negative. ELISAs for toxins A and B of C. difficile and for alpha, beta and epsilon toxins of Clostridium perfringens, respectively were negative. Salmonella culture and PCR were negative on colon tissue. Aerobic culture of liver and lung grew small numbers of Streptococcus equi ssp. zooepidemicus and mixed flora.
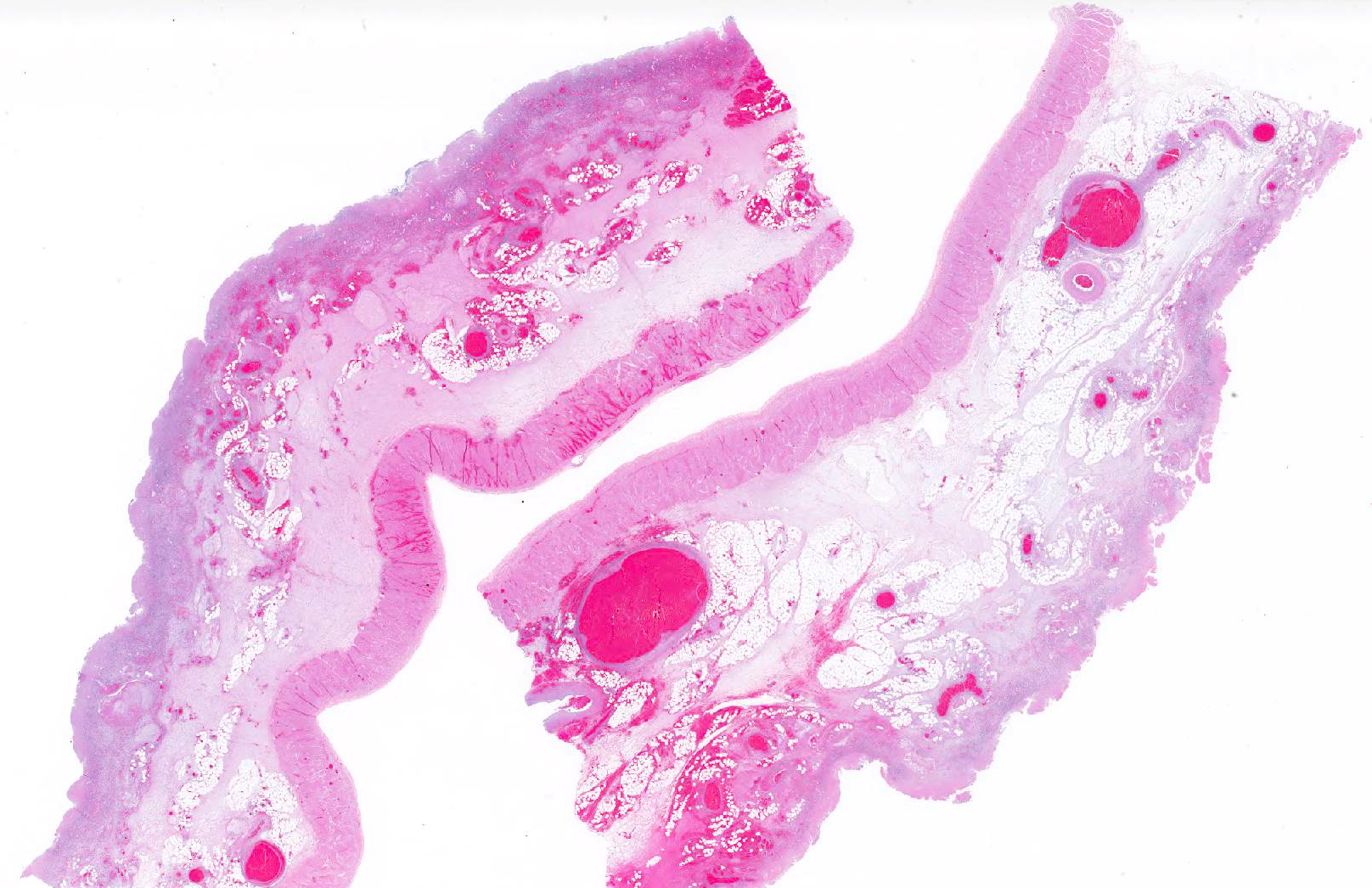
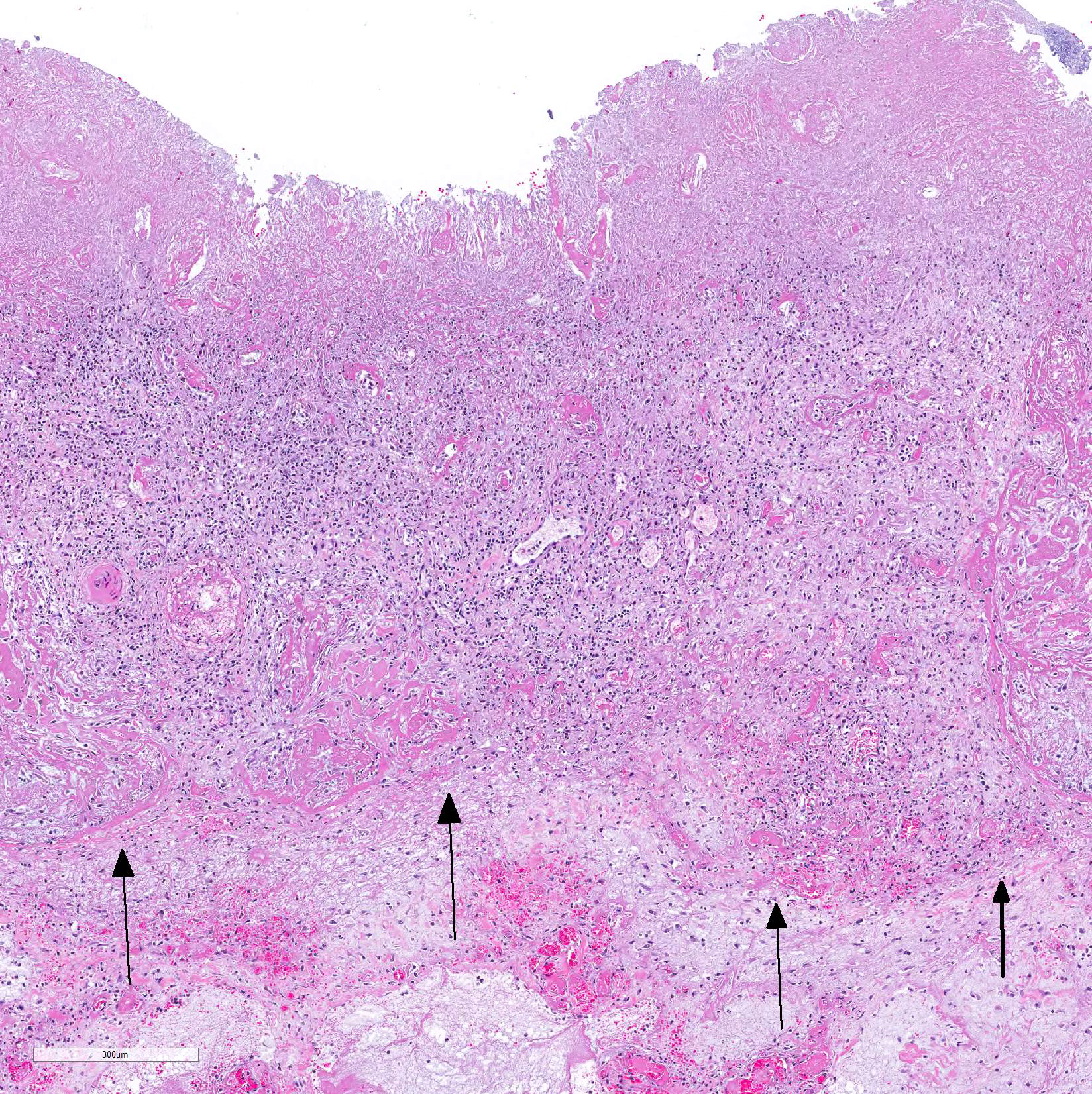
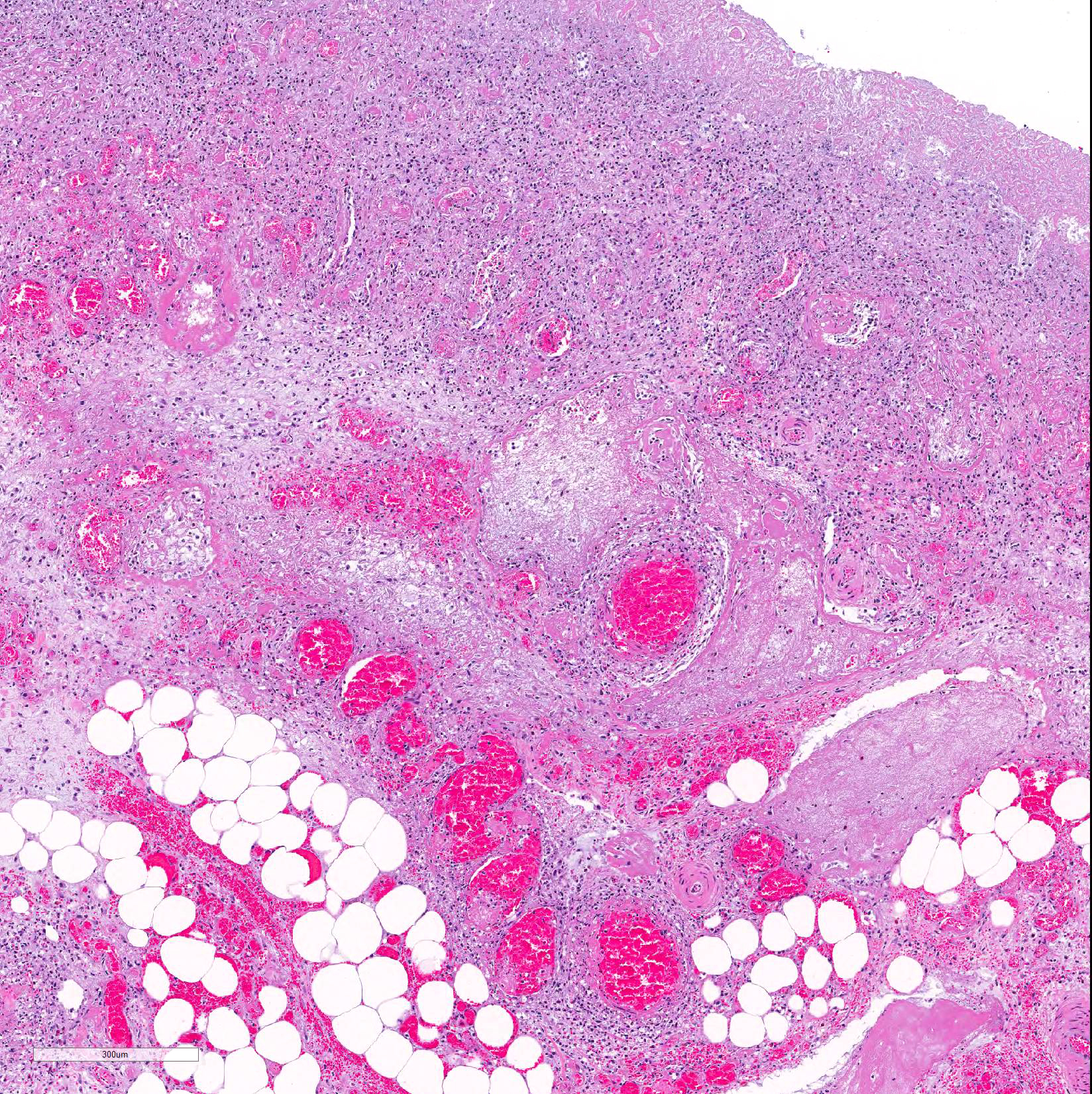
Microscopic Description: Colon: Diffusely, there is transmural congestion, edema and hemorrhage. The whole thickness of the mucosa is necrotic and presents lymphoplasmacytic and neutrophilic infiltration. The mucosal and sub-mucosal vasculature presents fibrin thrombi and thrombotic vessels show fibrinoid necrosis and infiltration with viable and degenerate neutrophils. These vessels are frequently surrounded by hemorrhage and viable and degenerate leukocytes. The sub-mucosa is greatly expanded by homogeneous eosinophilic edema and diffuse infiltration of lymphocytes, plasma cells, macrophages and neutrophils. The lymphatic vessels are dilated and contain large amounts of fibrin, red blood cells and neutrophils, both viable and degenerate. Large numbers of mix bacteria admixed with fibrin and cell debris cover the denudated superficial mucosa. The serosal blood vessels are also thrombotic and present fibrinoid necrosis.
Contributor Morphologic Diagnosis:
Colon, right dorsal: Colitis, severe, diffuse, acute, necrotizing with severe fibrinonecrotizing vasculitis, fibrin thrombosis and massive submucosal edema and congestion
Contributor Comment: Microscopic examination confirmed severe necrotizing right dorsal colitis with extensive vasculitis and many fibrin thrombi. Given the morphologic diagnosis, location, exclusion of C. difficile, C. perfringens and Salmonella spp., and history of banamine administration, this is likely consequence of nonsteroidal anti-inflammatory drugs (NSAIDs) toxicity.3,8
NSAIDs cause ulceration of the small intestine and colon in horses and other animals. In horses, even low doses of phenylbutazone can cause ischemic damage to the intestinal mucosa.8 Stress and/or dehydration are considered contributory factors to the pathogenesis of this condition.8 Because the right dorsal colon is preferentially involved, the condition is usually named ?right dorsal colitis?; however, lesions in other parts of the colon and in the small intestine may also occur.4,6,7 The pathogenesis of this condition is associated with decreased production of prostaglandin E2 and nitric oxide. Decreased prostaglandin is due to NSAID inhibition of cyclooxygenase 2 (COX-2).8
Morphologically, right dorsal colitis cannot be differentiated from some of the most common infectious colitis of horses (e.g. C. difficile, C. perfringens and Salmonella spp. infections). There are no specific tests to confirm the diagnosis of NSAID?s toxicity, and the diagnosis should therefore be based on a history of NSAIDs administration and ruling out infectious causes of colitis. While location of the lesion in the right dorsal colon helps to establish a diagnosis of NSAIDs toxicity, it should be kept in mind that these drugs can also affect other parts of the alimentary canal in horses.8
Contributing Institution:
California Animal Health and Food safety Laboratory system, San Bernardino branch, University of California, Davis.
JPC Diagnosis: Colon: Mucosal necrosis, diffuse, with mucosal and submucosal vasculitis and thrombosis, and severe submucosal edema.
JPC Comment: Since the mid -1980?s, overuse of non-steroidal anti-inflammatory drugs has been associated with a variety of lesions in horses, to include ulceration of various segments of the gastrointestinal tract, as well as papillary necrosis in the kidney and vascular damage in multiple organs.2 Hypovolemia has been shown to potentiate their anti-prostaglandin effects, making their usage particularly hazardous in horses with endotoxemia or colic. The published toxic dose for phenylbutazone in the horse is 8.8 mg/kg BW5 while in hypovolemic animals it is lowered to 6.0 mg/kg BW1.
Gastriointestinal ulceration may be seen at a number of sites in the GI tract with either aggressive NSAID use, to include the mouth, esophagus, and glandular stomach. While the particularly susceptibility of the right dorsal colon is largely unknown, a number of theories have been advanced but not proven. The slow transit time and proximal narrowing as it enters the small colon may allow increased mucosal contact time for orally dosed NSAID bound to feed particles. to include increased mucosal contact time with NSAIDs bound to feed in this slow-moving section of the gut, which also abuts a narrowing section in its connection to the small colon. Concentration gradients within the dorsal colon may also play a role, as the dorsal colon differs from the ventral colon in that fluid may be secreted as well as absorbed.1
Both acute and chronic syndromes
of right dorsal colitis have been described, with horses with acute disease
manifesting with colic, diarrhea, fever, depression, and shock. More chronic
disease, resulting in intermittent colic with weight loss, soft but not
diarrheic feces and ventral edema. Hyproproteinemia and hypoalbuminemia was
commonly seen in both acute and chronic presentations, with more severe levels
and panhypoproteinemia seen in cases with more chronic courses.2
At necropsy, areas of ulceration may be interrupted by islands of
regenerating mucosa, and in chronic cases, colonic submucosal fibrosis, stenosis
and impaction may be evident.2
References:
1. Galvin N, Dillon H, McGovern F. Right dorsal colitis in the horse: minimreview and reports on three cases in Ireland. Irish Vet J 2004; 57(8): 467-473.
2. Karcher LF, Gill SG, Anderson WI, King JM. Right dorsal colitis. J Vet Int Med 1990; 4:247-253.
3. Jones SL, Davis J, Rowlingson K. 2003. Ultrasonographic findings in horses with right dorsal colitis: five cases (2000?2001). J Am Vet Med Assoc 222:1248?1251.
4. Marshall JF, Blikslager AT. 2011. The effect of nonsteroidal anti-inflammatory drugs on the equine intestine. Equine Vet J Suppl 39:140-144.
5. Meschter CL, Gilbert M, Krook L, Maylin G, Corradino R. The effects of phenylbutaxone of the morphology of prostaganding concentras of the pyloric mucosa f the equine stomach. Vet Pathol 1990; 27:244-253.
6. Parfitt JR, Driman DK. 2007. Pathological effects of drugs on the gastrointestinal tract: a review. Hum Pathol 38:527-536.
7. Rotting AK, Freeman DE, Constable PD, Eurell JA, Wallig MA. 2004. Effects of phenylbutazone, indomethacin, prostaglandin E2, butyrate, and glutamine on restitution of oxidant-injured right dorsal colon of horses in vitro. Am J Vet Res 65:1589?1595.
8. Uzal FA, Plattner BL, Hostetter JM. Alimentary system. 2016. In: Maxie G ed., Jubb, Kennedy and Palmer?s Pathology of domestic animals. Vol. 2, pp. 1-257. Elsevier, St. Louis, MO.